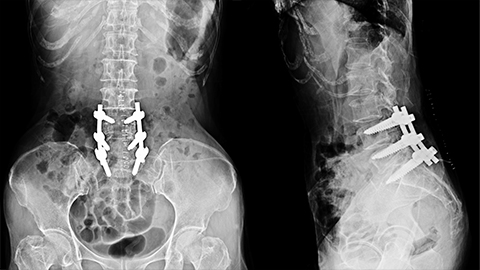
A client has chronic low-back pain, headaches, migraines, and a history of some serious surgeries. We take a close look at one of them: spinal fusion at L4-L5. What is this massage therapist doing now? What might he do in the future? It turns out there are a lot of options!
Case study of a client with a spinal fusion:
- Keller, G. (2012). “The Effects of Massage Therapy after Decompression and Fusion Surgery of the Lumbar Spine: A Case Study.” International Journal of Therapeutic Massage & Bodywork, 5, no. 4, 3–8. www.ncbi.nlm.nih.gov/pmc/articles/PMC3528189/.
Information on spinal fusion procedures:
- https://orthoinfo.aaos.org/en/treatment/spinal-fusion/
- https://www.spine-health.com/treatment/spinal-fusion/lumbar-spinal-fusion-surgery
Video
Selected research on massage therapy and scar tissue:
- Ault, P., Plaza, A., and Paratz, J. “Scar Massage for Hypertrophic Burns Scarring—A Systematic Review.” Burns: Journal of the International Society for Burn Injuries 44, no. 1 (2018): 24–38. https://doi.org/10.1016/j.burns.2017.05.006.
- Shin, T. M., and Bordeaux, J. S. (2012). “The Role of Massage in Scar Management: A Literature Review.” Dermatologic Surgery: Official Publication for American Society for Dermatologic Surgery [et al.], 38, no. 3, 414–23. https://doi.org/10.1111/j.1524-4725.2011.02201.x.
Continuing education on massage therapy and scar tissue:
- Scar Tissue Management (3-part series)
- Scar Management: Principles, Practice, and Protocol (The Beginning)


This podcast sponsored by Books of Discovery and Anatomy Trains.
00:00 Speaker 1: Ruth Werner's best-selling book, A Massage Therapist's Guide to Pathology, is a highly regarded comprehensive resource that sets the standard for pathology education. Written for massage therapy students and practitioners, this groundbreaking resource serves up a comprehensive review of the pathophysiology signs, symptoms and treatment of more than 500 diseases and disorders. Learn more at booksofdiscovery.com.
[music]
00:39 Speaker 2: Hi, and welcome to, I Have A Client Who... Pathology conversations with Ruth Werner, the podcast where I will discuss your real life stories about clients with conditions that are perplexing or confusing. I'm Ruth Werner, author of A Massage Therapist's Guide to Pathology, and I have spent decades studying, writing about, and teaching about where massage therapy intersects with diseases and conditions that might limit our client's health. We almost always have something good to offer, even with our most challenged clients, but we need to figure out a way to do that safely, effectively, and within our scope of practice, and sometimes, as we have all learned, that is harder than it looks. This week's podcast will focus on a client with some complicated problems, some of which may be helped by massage therapy. It comes from a massage therapist in Texas who shares this story. "I have a client who is a nurse in her 40s, who has really bad low back pain. She had a fusion at L3-L4. To me, her spine looks completely straight, no lordotic or kyphotic curves at all. She has a lot of residual scarring from her surgery, and to make things even more complicated, about three or four years ago, she donated a kidney."
02:02 S2: Here's what an amazing person she is. She heard a story about a kid who needed a kidney and she found out she was a match and she just gave her kidney away, and that surgery involves a big incision and a lot of scar tissue and many lifestyle modifications. It was interesting that her low back pain was not worsened by her surgery. On top of what was already going on with her low back, all that scar tissue made working with her, a special challenge, she always has complaints of headaches and migraines every time she comes in. This person is the reason why I pursued so much continuing education, especially about working with low back and hips, she gets some relief when I try to create some space in her low back with traction on the sacrum and some stretching of the psoas muscle. I'm happy to say, she finds that getting massage makes her feel better and she uses pain meds only as a last resort. As always, I wanna offer my deep gratitude to the massage therapist who shared this story of his amazing client. If you have a story about an amazing client, or even just a story about a question that came up as you're working with your clients and you're wondering if you're on the right track, be sure and let me know, at ihaveaclientwho@abmp.com. That's ihaveaclientwho, all one word, all lowercase, @abmp.com.
03:35 S2: Well, there are so many different directions we could go with a short discussion of this client. We could talk about what it means to donate a kidney because that's a complicated undertaking, but I think we'll make it other requests for podcasts about donating or receiving transplanted organs, so we'll hold off on that for now. Instead, let's home in on this client's history of spinal fusion surgery, and then we can also talk a little bit about massage and scar issue. I have never written or read extensively on spinal fusion surgeries, but after what I looked at today, that might change. As I dug around a little bit to gather some information for this podcast, I am finding all kinds of fascinating information about this process. For instance, spinal fusion surgeries place a piece of natural or synthetic bone and they graft it in between the vertebral bodies, and then this craft is stimulated so that the connecting bones grow and fuse all into a single unit. The goal, of course, is to maintain appropriate space between the vertebrae, so we don't have nerve pressure that generates pain, spinal fusions are done in the neck or in the lumbar spine, not usually in the thoracic spine, because of course, the ribs stabilize us there.
05:00 S2: One of the consequences of spinal fusion surgery, which is a very complicated surgery with a lot of risks and hazards involved, is that while we address those bones that are problematic and they become extremely well stabilized because essentially, they form single bones. This is gonna put an increasing demand on the joints, both above and below where the fusion is, because remember, every joint in our spine, both at the cartilaginous side on the anterior aspect and between the vertebral facets on the posterior aspect, every joint between those bones is meant to have at least a little bit of freedom of movement, and when you add up all the movement between the stepped vertebrae, of course, then we get our typical spinal range of motion, which allows us to flex and extend and side flex and rotate and all the things that we love and need to do with our spines. So this client had a fusion at L4-L5, and what this means is she probably had either a pretty severe case of degenerative disc disease that other interventions were not helping with, or she might have had another condition called Spondylolisthesis, where. You wanna say that with me? Spondylolisthesis.
06:22 S2: And in this situation, some structural changes in the lumbar vertebrae allows the vertebral body to sort of slip anteriorly, and this can create a lot of kinds of problems. People, sometimes will have a spinal fusion surgery after a really severe trauma or to treat super severe scoliosis, but most of the time it's related either to a chronic disc problem or this spondylolisthesis situation. Regardless, when we have bones in the spine that are not in the correct position, then they can exert pressure on nerve roots or on the spinal cord itself, and the results can be chronic, predictable, un-remitting pain and even loss of nerve function and loss of bladder and bowel control, if the spinal cord itself is disrupted, and obviously we would rather that didn't happen. Now, it's appropriate to try virtually every other option we can think of before settling on a spinal fusion surgery. And I think it's probably safe to say that there have been periods in time when people have taken a surgical route, maybe prematurely without trying other less invasive options that might have been more successful.
07:42 S2: In the world of pain science, and where we look at pain in the bio-psycho-social context, the bio-part of that triad refers to mechanical disruptions like nerve pressure from discs or bone spurs or whatever. But we also know that someone who lives with chronic pain, especially pain that really interferes in their ability to get through their day, well, these folks are also vulnerable to subtler and sometimes harder, more stubborn versions of pain related to psychosocial issues. For instance, living in pain may cause them to retreat from their relationships, and we see that people who live in isolation deal worse with health issues than those who have a supportive community. And all this is the long way around of saying that for someone who has lived with chronic pain, surgery may be a useful and effective option, but it's probably not the only useful and effective option that someone might need. I looked up success rates for spinal fusion surgeries and from spine-health.com, I learned that spinal fusion surgeries improved pain usually by 60% to 70% for most patients, so most people don't have a complete resolution of their pain, but about 80% of patients say that they are satisfied with their outcomes. In other words, that the surgery was probably the right choice for them. So this client evidently had a pretty successful outcome with her surgery since she continued to be a nurse and was able, several years later, even to donate a kidney.
09:20 S2: However, as this massage therapist points out, she appears to have lost some of that balance that curves allow us to provide in our spine. His observation was that her lumbar curve and her kyphotic curves were completely diminished and her spine looked sort of like a tent pole rather than like the curvy spine that allows us to have shock absorption and balance. So it's not surprising with that phenomenon that she's reporting headaches and migraines, along with her chronic low back pain. This massage therapist says he gets pretty good results when he focuses on elongating her lumbar curve with sacral traction and stretching the psoas. This sounds like good strategies, as long as whatever he's doing to position her on the table doesn't threaten anything to do with her fusion, but we don't have from this information how long ago her surgery was.
10:19 S2: Yeah, but that said, based on everything we've been talking about so far, it seems safe to assume that it predated her coming to see him as a client. So I'm not in current practice, and I don't usually give advice about techniques. This therapist has been motivated by this client to pursue continuing education to work with low back pain, and I think that's awesome. It's terrific. In addition though, I would love to see him and massage therapists who have clients with similar complicated surgical histories, maybe to look at some advanced education in the field of working with scar tissue. I think it's probably not accurate to say that massage therapy breaks up scar issue or breaks down scar tissue or even releases scar tissue, but I think it is realistic to suggest that careful skilled massage therapy could improve the quality of scar tissue in terms of its playability, it's flexibility and the experience and function of the person who's living with it. And this would be true both for scarring related to this client's fusion surgery and the very extensive scarring that can go along with being a kidney donor.
11:34 S2: Guess what I found, I found a case report published by the International Journal of Therapeutic Massage and Body Work, and here's the title, The Effect of Massage Therapy After Decompression And Fusion Surgery of a Lumbar Spine, A Case Study. Of course, I will put the link to this free full text, open sourced scientific journal article, specifically about massage therapy in our show notes today, but I will let you know that in this case study, the client was a 47-year-old woman who underwent this surgery at L4-L5, just like our podcast client due to chronic disc herniation symptoms, and the goal was to see if massage therapy could help treat her pain and dysfunction that's associated with this kind of surgery. They had some success, especially around things to do with a range of motion and hamstring length. They also used a disability index to measure her sense of her ability to function, and they did some pain scores that showed some improvement in her pain scores as well, and overall they had a good experience with a limited number of massages over a specific period of time. Now, our own client's goals could be really different from the goals of the client in this published case study, but when we do a quick search for things like this, it puts us a giant step forward in figuring out how to best provide evidence-informed practice and how to not keep reinventing the wheel if we don't have to.
13:15 S2: While I was at it, I took a quick look at pubmed.gov, looking for research about massage therapy in the context of scarring, including post-surgical scarring and burn-related scarring, and there's a lot of data. I didn't look at it in detail, that's your job when you have clients who fit these descriptions, but I will put some links of two titles that I thought were especially interesting in the show notes. I also know that there are some really outstanding continuing education classes in working with various types of scar tissue and other connective tissue constriction problems, so I'll post a few options. And you may have others that you like as well, and maybe you could share them in the comments. So here's the wrap-up to this situation, this massage therapist wants to bring his best to this client who has low back pain and lots of scar tissue and chronic headaches and migraines, and he's helped her with her pain by working to help her decompress her lumbar spine, but it seems clear that there's more work to do. Fortunately, there are a lot of options he can pursue, by looking for advanced education in dealing with scar tissue, and by looking at what other massage therapists have done with similar kinds of problems.
14:38 S2: The moral of the story for me is that when you hit a dead end with your client and you're not making the progress that you'd like to make, don't stop there. Look around for some other options because there may be some great ones just waiting for you to find them. Hey everybody, thanks for listening to I Have A Client Who, pathology conversations with Ruth Werner. Remember, you can send me your, I Have A Client Who, stories to ihaveaclientwho@abmp.com. That's ihaveaclientwho, all one word, all lowercase, @abmp.com. I can't wait to see what you send me, and I'll see you next time.
15:24 S1: Anatomy Trains is excited to announce a new on-demand video course with Tom Myers coming soon; deeper ground, restoration and vitality for the female pelvis. Reach your deeper ground of embodied awareness and strategic confidence with this four-hour tour of the female pelvis, including its key points and unique challenges. Course highlights include hands-on, palpation certainty and technique review for the major muscle groups, assessments and techniques for posterior and anterior pelvic floor, psoas complex and diaphragm, common perinatal bio-mechanical issues explained and much more. Sign up for the Anatomy Trains newsletter at anatomytrains.com to be notified when the course is available.