By Ruth Werner
We’re not done with COVID, not by a long shot (public behavior notwithstanding), but a lot of focus has shifted to another infectious disease making a big impact this summer—monkeypox.
I put together some information in mid-July on this topic, but it's time for an update.
What Is It?
Monkeypox is a viral infection. It is a member of the Orthopoxvirus family, along with smallpox and cowpox.
The name “monkeypox” is a bit misleading. It was first identified in monkeys in 1958, and in humans in 1970, but it occurs most often and is spread to humans most easily by a variety of rodents. Animals that can carry this virus include prairie dogs, squirrels, and groundhogs, but it has also been seen in other mammals. It may affect certain varieties of domestic rabbits, mice, and rats. We don’t know whether other common household pets like gerbils, guinea pigs, and hamsters can spread monkeypox.
Monkeypox is similar enough to smallpox that anyone vaccinated against smallpox has protection from monkeypox, which is good news for some of us. The worldwide campaign to vaccinate against smallpox was so effective, however, that the virus was essentially eradicated in the wild, and routine vaccination in the US was suspended in 1972. That means people under 50 years old probably have not been vaccinated for smallpox, so they lack protection from monkeypox.
Epidemiology?
Until recently, monkeypox outbreaks were geographically limited to Central Africa (one subtype or “clade” of the virus that is highly virulent), and to West Africa (a different, less virulent clade). In Central Africa especially it can be a serious health threat, with infections severe enough to cause death in 3–10 percent of diagnosed cases. Ironically, some effective vaccines against this virus have been developed, but they are not made available to African populations who need them most.
Statistics in mid-July 2022
Over 10,000 cases of monkeypox have been reported this year. In addition to parts of Africa where this infection has been seen before, these have occurred in Europe, Asia, South America, North America, and Australia—all places where monkeypox is not typically seen. The US has seen 866 confirmed cases so far, and that number is rising quickly. No deaths from this infection have been reported outside of Africa at this point.
Statistics in late-August 2022
Worldwide, the current confirmed case count for Monkeypox is 46,744; and over 46,000 of those cases are outside of Africa. The U.S. has confirmed 16,926 cases. Deaths have occurred in Brazil, Ecuador, Cuba, India, and Spain, as well as in African countries. However, this is not a typical outcome; only 13 deaths related to monkeypox have been reported around the world this year. Also in at least some of the cases the deaths occurred in people who were severely immune compromised.
Also it’s worth noting that in many countries new monkeypox infections appear to have peaked and are now subsiding. The U.S. numbers have also been falling since early August, but this is a trend that we should watch carefully, because it could certainly change.
Signs and Symptoms
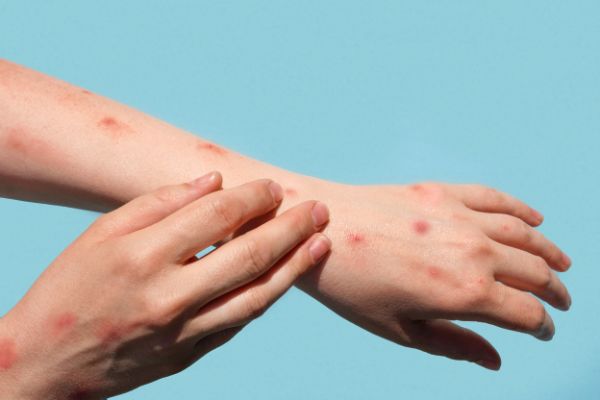
In its most typical form, monkeypox infections typically incubate for 1-2 weeks after exposure. Then patients may develop fever, malaise, and inflamed lymph nodes; this is the prodrome stage. This is followed by a painful rash with blisters that then fill with pus, and eventually become itchy as they scab over and heal over a course of 2-4 weeks. The rash may be all over the body or local to the site where the infection was contracted. However, some people don’t experience the prodrome stage with fever and inflamed lymph nodes: their first symptoms are the characteristic blisters, which can range from being mild to excruciatingly painful.
The less virulent form of monkeypox is a self-limiting infection: it runs its course and then resolves without life-threatening complications if the patient is healthy to begin with. However, it can cause substantial and long-lasting pain in some patients. And in people who are immune-compromised, it may cause central nervous system infections that can be dangerous or deadly.
Transmission
Historically, monkeypox has been spread from infected animals to humans through close contact, bites and scratches, or through preparing an animal for consumption.
Human-to-human spread is a new phenomenon. It occurs through direct, often intimate or sexual, contact with a symptomatic person, or through prolonged contact with their bedding, clothing, or other intimate items—these are fomites. Researchers believe it may also be spread through respiratory droplets, as well as by way of contact with infected skin lesions. It is communicable from the onset of symptoms through when the skin lesions are fully healed, which can take several weeks.
The public health community is working to discover how easily monkeypox virus can be spread through asymptomatic shedding from an infected person. Some evidence suggests this is possible, but not common: at this point most cases are related to prolonged skin-to-skin contact or skin-to-fomite contact.
Treatment
As a viral infection, monkeypox can’t be treated with antibiotics. No antiviral medications have been officially approved for it, but some have been provisionally used in the absence of other options, and testing is underway for others. But getting through monkeypox is usually a matter of time: from exposure to prodrome fever and swollen lymph nodes through the rash and healing of the lesions.
So far, this infection has usually been mild and self-limiting. Infected people are counseled to isolate, and others in their circle may qualify for vaccination to help limit community spreading.
Two vaccines against monkeypox are available in the United States. They are distributed through local health authorities who may place priority on holding vaccines for people who are most at risk.
Implications for Massage Therapy
What does all this mean for our practice? We know a few things about monkeypox that can help us feel confident about our clinical decisions, at least until information changes.
The main issue to keep in mind is that while the practice of massage therapy involves touch and close contact, this infection does not appear to be easily communicable in asymptomatic people. If our clients have fever, malaise, and swollen lymph nodes, they need to delay their massage—that is true in all cases, not just for monkeypox. If our clients have undiagnosed blisters, pustules, or scabs that started as blisters, they should investigate this with their primary health-care provider before receiving massage. Again, this is true for all circumstances, not just monkeypox. Consider adding the following question to your intake form: Do you have any blisters or pimples in a new pattern?
Because it is possible that respiratory droplets may carry some virus, it is important to continue to observe excellent hygienic practice in massage settings.
Finally, if a massage therapist is working in an area where monkeypox is very prevalent, they might think about using gloves during massage, until numbers subside and monkeypox is no longer considered a significant risk.
In short, if we follow basic precautions about working with people who don’t have signs of communicable diseases, clients with communicable monkeypox will most likely not find their way to our table.
How long after an infection should we wait to offer massage? Experts agree that after the rash has fully healed (that is, the blisters have scabbed, and the scabs have fallen off), the person is no longer contagious. That may take several weeks, but it is at least a clear guideline.
I hope this overview of monkeypox has helped you feel more confident and capable of dealing with this possibility in your practice. Once again, information is our best defense, and now you have some resources you can use to keep yourself and your clients safe.
author bio
Ruth Werner is a former massage therapist, a writer, and an NCBTMB-approved provider of continuing education. She wrote A Massage Therapist’s Guide to Pathology (available at BooksofDiscovery.com) now in its seventh edition, which is used in massage schools worldwide.
Resources
Bajaj, Simar. SmithsonianMag.com. “What You Need to Know About the History of Monkeypox.” June 24, 2022. www.smithsonianmag.com/history/what-you-need-to-know-about-the-history-….
Centers for Disease Control and Prevention. “2022 Monkeypox Outbreak Global Map.” Accessed July 2022. www.cdc.gov/poxvirus/monkeypox/response/2022/world-map.html.
Centers For Disease Control and Prevention. “Interim Clinical Considerations for Use of JYNNOES and ACAM2000 Vaccines During the 2022 U.S. Monkeypox Outbreak,” Updated August 22, 2022. www.cdc.gov/poxvirus/monkeypox/considerations-for-monkeypox-vaccination….
Centers for Disease Control and Prevention. “Monkeypox in Animals.” Updated August 17, 2022. www.cdc.gov/poxvirus/monkeypox/veterinarian/monkeypox-in-animals.html.
Kozlov, Max. “Monkeypox in Africa: The Science the World Ignored.” Nature 607 (2022): 17–18. https://doi.org/10.1038/d41586-022-01686-z.
National Institute of Allergy and Infectious Diseases. “Monkeypox Treatment.” Content last reviewed August 21, 2022. www.niaid.nih.gov/diseases-conditions/monkeypox-treatment.
Scherer, Liz. Medscape.com. “Monkeypox Fatalities Reported as Cases Escalate.” August 2, 2022. www.medscape.com/viewarticle/978431.
Schnirring, Lisa. Center for Infectious Disease Reasearch and Policy. “Study Heightens Concerns About Asymptomatic Monkeypox Spread.” August 16, 2022. www.cidrap.umn.edu/news-perspective/2022/08/study-heightens-concerns-ab….
Related Content:
ABMP members: Find your client health intake forms here.
ABMP Pocket Pathology is a quick-reference app exclusively for ABMP members that puts key information for nearly 200 common pathologies at your fingertips. ABMP Pocket Pathology lets you go into your sessions armed with the knowledge necessary to make the best treatment decisions for your clients, and it’s easy to use, whether you’re accessing it from your phone or laptop.