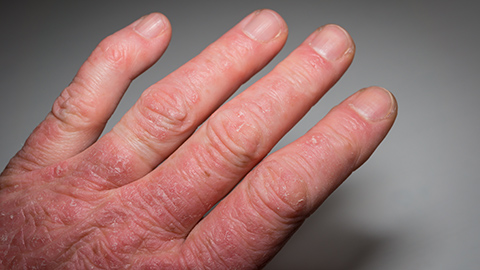
A massage therapist is in a rather severe bike accident, being hit by a vehicle—on purpose. In addition to his other injuries, he develops a sudden onset of episodes of skin lesions and severe joint pain that persists to this day. What in the world is going on here, and what can he do about it? This is an inspiring story of remarkable resilience.
General information on psoriatic arthritis:
Video:


This podcast sponsored by Books of Discovery and Anatomy Trains.
00:00 Speaker 1: Ruth Werner's best-selling book, A Massage Therapist's Guide To Pathology, is a highly regarded comprehensive resource that sets the standard for Pathology Education, written for massage therapy students and practitioners. This groundbreaking resource serves up a comprehensive review of the pathophysiology, signs, symptoms and treatment of more than 500 diseases and disorders. Learn more at booksofdiscovery.com.
[music]
00:39 Ruth Werner: Hi, and welcome to, I Have A Client Who... Pathology conversations with Ruth Werner, the podcast where I will discuss your real life stories about clients with conditions that are perplexing or confusing. I'm Ruth Werner, author of A Massage Therapist's Guide To Pathology, and I have spent decades studying, writing about and teaching about where massage therapy intersects with diseases and conditions that might limit our client's health.
01:08 RW: We almost always have something good to offer even with our most challenged clients, but we need to figure out a way to do that safely, effectively and within our scope of practice, and sometimes, as we have all learned, that is harder than it looks. This episode is going to be a little bit different from some of our others, because our client on whom we are focusing is not a client, it is a massage therapist, but this person had a really interesting and compelling story to share, and so that's what we're going to do. It goes like this. I am a massage therapist who was hit by a vehicle while training for a triathlon on my bike at the age of 24, and along with all the other injuries, it triggered an autoimmune reaction. I developed some kind of mysterious arthritis in my shoulders, my elbows, my knees, my ankles and my hands. All my joints pop and crack and make a lot of noise, it would be really hard to sneak up on someone. Four months after my incident, I even broke out with shingles, tracing from my right armpit all the way down to my wrist. I would definitely rather get hit by a car again than get shingles, just saying.
02:25 RW: Much later, I had outbreaks of Psoriasis. That helped my doctors decide I had Psoriasis Arthritis. It usually goes in the opposite order, with Psoriasis first and arthritis later. I live in pain all the time. Mostly it's around a three, but on bad days, it flares to seven to eight, sometimes the flare-ups in my back and rib cage gets so bad, it can be hard to breathe deeply. I get these internal joint pains where it feels like I broke my bones followed by swelling for a few days, and then it comes back down. When I'm well enough, I run and eat healthily, I get massages every week. I also use flotation therapy to help reduce swelling and decompress my joints, but the salt water in the psoriatic lesions can sting a little when I'm just getting in. It goes away pretty quickly. The salt water actually helps reduce my Psoriasis and eczema, those lesions look like they're closed, but they're not. The visible lesions are all over my body, including up over my scalp, but they are not my main problem though, it's really the joint pain. I tried a couple of immune suppressant treatments, but they just made me feel awful and they didn't seem to help. I wanna stay off them if I can, so I make a consistent effort to live a healthier lifestyle, including massage and proper diet and exercise and sleep. I can still teach massage, but it's hard for me to give massage for an hour at a time. I own a spa, and that's the main way I stay involved in practice now.
03:57 RW: What a story. I happen to know a little more about this massage therapist, and it's even more dramatic than it sounds. His bike accident was no accident, he was intentionally hit, and it was only by the merest chance that he survived without devastating injuries. As it was, he was out of commission for three months while he recovered. I wanted to bring this story to I Have A Client Who... Because the relationship between Psoriasis and Psoriasis Arthritis is really interesting, and because Psoriasis is pretty common, but a lot of people have never even heard of Psoriasis Arthritis. But before we continue, I wanna make sure to invite you to submit your, I Have A Client Who's stories. You can do that by sending them to me at ihaveaclientwho@abmp.com, that's, I have a client who, all one word, all lowercase, at A-B-M-P dot com.
04:58 RW: So let's talk about Psoriasis. This word comes from the Greek, and it means itch, condition of itch. This is kind of interesting because if you have Psoriasis, you know this, I used to get it every now and then, the lesions themselves are a little bit itchy, but they're not super itchy like we would see, say with scabies or insect bites or other kinds of irritation. When I first started learning and teaching about pathology, Psoriasis was considered to be just an idiopathic skin condition, we now consider it to be autoimmune, and that makes a lot of sense, because it has a lot in common with a bunch of other autoimmune conditions. It appears in cycles of flare and remission, and it frequently appears in conjunction with certain other diseases like, Ankylosing Spondylitis and a couple of other autoimmune things. Specifically, these are called seronegative autoimmune diseases, because they don't show specific blood markers. So they're often diagnosed in the absence of blood markers that would indicate other kinds of problems.
06:04 RW: So what happens with Psoriasis is that in isolated patches on the skin, the production of new skin cells is vastly accelerated. You might remember that normal skin cell production takes place on a roughly 28-day cycle, which might make you go, "Huh, there's another 28-day cycle I can think of." So typically, we are pushing up new skin cells all the time, and about every month or so, every skin cell has been replaced. But with Psoriasis, this is accelerated to take maybe three or four days instead of 28 days, but in these isolated patches. So we get these pileups of new skin cells and they're growing up from the deepest layers of the epidermis out toward the surface, but before those surface cells are really ready to slough off. So what this looks like is reddish or pinkish patches on the skin, and they might be covered by white flaky skin. If they last for a long time, they develop a sort of silvery scale and these long-term lesions can also contract in on themselves, and that makes the skin look scarred.
07:14 RW: What I've just described here is called Plaque Psoriasis, this is the most common form and it's the version that our contributor today, lives with. There are other forms of Psoriasis. But they're much less common. One of the things that most massage therapists are really glad to learn about Psoriasis is that it is in no way contagious, we cannot catch it from clients. It's really fully related to internal processes. People who have Psoriasis tend to have more proinflammatory chemicals and an abnormally high number of a specific kind of immune system cell in the superficial fascia, these are called dendritic cells. And these dendritic cells stimulate T-cells and they secrete inflammatory chemicals, and the whole thing leads to this hyperactivity at the basal layer of the skin.
08:04 RW: If you think about it, this accelerated production of cells in an isolated area, what does that sound like? To me, it sounds like cancer cells and cancer growth, but in fact, I have never seen anyone make a case that there's any kind of correlation, statistical or otherwise, between Psoriasis and a risk for skin cancer. It's just interesting to see that our bodies do not thrive when our cell-making apparatus gets overactive. Psoriasis can be treated with topical antiinflammatories, but most people find this is not that effective. Are these new discoveries about how the immune system works to create this problem have led to some new treatment options that affect immune system responses, still, this is a really challenging condition to treat. Most people find that one treatment option for these skin breakouts will work for a while and then it won't work anymore and they have to switch to something else. And sometimes these treatment options conflict with each other to make some dangerous side effects, the whole thing can create a serious challenge to try to get on top of it. Psoriasis is common. It affects up to seven and a half million people in the United States.
09:19 RW: When it's pretty mild, we might see it on elbows or knees, that's a really typical kind of presentation. But some people have it in a very severe way and it can cover their trunk, the palms of their hands, the soles of their feet, and go up even under the scalp, and this is the form that affects our contributor today. His bouts with Psoriasis or whole body episodes. In addition, he has now developed a complication that we see in around 10 to 30% of patients who have Psoriasis, and this is something called Psoriasis Arthritis, but he did it in a backwards order. His first symptoms were of Psoriasis Arthritis and his skin episodes of Psoriasis didn't appear until later. So Psoriasis Arthritis is joint inflammation that is related specifically to this autoimmune attack on our own tissues. When it occurs at the spine, it can look a lot like Ankylosing Spondylitis. Remember, that's one of the autoimmune diseases that is frequently seen alongside Psoriasis. When Psoriasis Arthritis occurs in the extremities, it looks a lot like rheumatoid arthritis. There are a few subtypes of Psoriasis Arthritis, and I found a nice video that offers a pretty succinct overview of this condition, so I'll be sure to include a link to that in our show notes for today.
10:44 RW: One thing that makes both Psoriasis and Psoriasis Arthritis really different from other autoimmune diseases, is they have a funny pattern, in that they often develop after some kind of major physical trauma, and we don't see this with many other conditions outside of things like Fibromyalgia or Chronic Fatigue Syndrome. So an episode of Psoriasis following some kind of physical trauma happens so predictably, it has a name, it's called The Koebner Phenomenon, and given this massage therapist's experience, it's clear that his bicycling incident was the trigger for his autoimmune flare. The treatment options for Psoriasis Arthritis are similar to what we see for other autoimmune types of joint inflammation, and that means our guidelines for massage therapy are similar as well. In a nutshell, we need to avoid anything intrusive while the joints are inflamed and painful, and we must work within pain tolerance of course, but we can then focus on pain-free range of motion and the reduction of unnecessary muscle tension around painful joints when our client is in remission.
11:54 RW: Other general guidance would be related to our client's goals, of course. If you have clients who have Psoriasis or Psoriasis Arthritis, let me recommend that you take a quick peek at the resources I've provided with this podcast or your pathology book, because you will find useful information there. Remember our contributor said that his lesions, his skin lesions sting when he gets into his float tank, and that suggests that there are open lesions and a risk for secondary infection, this means active Psoriasis outbreaks are at least local contraindications, and if we're gonna work with someone who's living with this, it is best probably to work either with gloves or through the sheet so we can avoid any risk of creating a new infection.
12:40 RW: This massage therapist has shared with us what he can do when he's feeling well. He runs, he eats carefully, he gets lots of massage, he uses the flotation tanks at his spa, but it's clear there are times when he does not feel well enough to take care of himself, in this way. I've gotten to know this person a little bit in recent months, and I'm really glad that he is part of our Massage Therapy community. The way he's dealt with his challenges and obstacles has been really inspiring to me and to many others. I hope he continues in our profession, I hope he gets the support he needs to take really good care of himself, because his contributions can continue to inform us all.
13:23 RW: Hey everybody, thanks for listening to, I Have A Client Who... Pathology conversations with Ruth Werner. Remember, you can send me your, I Have A Client Who's stories to, ihaveaclientwho@abmp.com, that's, I have a client who, all one word, all lowercase, at A-B-M-P dot com. I can't wait to see what you send me, and I'll see you next time.
13:51 S1: Anatomy trains is excited to announce a new on-demand video course with Tom Myers coming soon, deeper ground, restoration and vitality for the female pelvis. Reach your deeper ground of embodied awareness and strategic confidence with this four-hour tour of the female pelvis, including its key points and unique challenges. Course highlights include; hands-on, palpation certainty and technique review for the major muscle groups, assessments and techniques for posterior and anterior pelvic floor, psoas complex and diaphragm, common perinatal bio-mechanical issues explained and much more. Sign up for the Anatomy Trains Newsletter at anatomytrains.com, to be notified when the course is available.