A client reports she has Sprengel’s deformity and was told never to get massage or chiropractic. Nonetheless, she finds that massage is very helpful!
What is Sprengel’s deformity? And what are the questions we need to ask so we can make safe and effective clinical decisions?
Spoiler alert: It’s not as tricky as it sounds, and you’ll find out on this episode of “I Have a Client Who . . .”
Resources: 
Pocket Pathology: /abmp-pocket-pathology-app
Kafadar, C. et al. (2016) ‘Omovertebral bone associated with Sprengel deformity presented with chronic cervical pain’, The Spine Journal, 16(2), p. e43. Available at: https://doi.org/10.1016/j.spinee.2015.09.044.
Köhler, S. et al. (2021) ‘The Human Phenotype Ontology in 2021’, Nucleic Acids Research, 49(D1), pp. D1207–D1217. Available at: https://doi.org/10.1093/nar/gkaa1043.
Sprengel’s Deformity - Pediatrics - Orthobullets (no date). Available at: https://www.orthobullets.com/pediatrics/4038/sprengels-deformity (Accessed: 15 February 2023).
Zarantonello, P. et al. (2021) ‘Surgical Treatment of Sprengel’s Deformity: A Systematic Review and Meta-Analysis’, Children, 8(12), p. 1142. Available at: https://doi.org/10.3390/children8121142.
Wikimedia, authors Stelzer, John W.; Flores, Miguel A.; Mohammad, Waleed; Esplin, Nathan; Mayl, Jonathan J.; Wasyliw, Christopher - Available at:
https://commons.wikimedia.org/wiki/File:Klippel%E2%80%93Feil_syndrome_and_Sprengel%27s_deformity.png


Massage Mentor Institute
In 2019, Diane Matkowski, aka the Massage Mentor, began a closed Facebook page for hosting discussions with industry leaders. These interviews gave her an idea for The Massage Mentor Institute and Jam Series workshops.
The goal was to create various continuing education classes offered in one spot. The Institute is a space for massage therapists to learn different approaches and philosophies of bodywork and business classes. It’s also home to the Shoulder, Hip, Neck, and Back Jam workshops.
We believe that no one technique works for every human being. Our goal is to help you find your path. We have selected teachers we trust, admire, and believe will help you grow as a licensed massage therapist.
Website: themassagementorinstitute.com
Facebook Group: facebook.com/themassagementor
Instagram: @massagementorinstitute
0:00:01.4 Ruth Werner: Hello I Have A Client Who listeners, Ruth Werner here and I'm so excited to let you know that my library of online self-paced continuing education courses has just expanded. I now have a two-hour ethics course called A Doctor's Note is Not Good Enough and What is Better. This NCBTMB approved course goes into why a doctor's permission or approval or even a prescription doesn't provide the legal or safety protection you might think it does. Then we look at how to start useful conversations with healthcare providers that will actually get us to safe and effective massage for our clients with complex conditions. Visit my website at ruthwerner.com for more information and to register for A Doctor's Note is Not Good Enough and What is Better.
0:00:52.9 Speaker 2: Introducing Back Jam, held online the first four Mondays in May, 2023, and hosted by the Massage Mentor Institute. This is the fourth event in a series of workshops focused on a single region of the body. We've gathered the following industry leaders, Till Lukau, James Waslaski, Tom Myers, Diane Lee, Paul Kelly, Sue Hitzman, Whitney Lowe, Aubrey and Alison Gowing, Allison Denny, Judith Astin, Benny Vaughn, Heath and Nicole Reed, and Ruth Werner. Sign up for the Back Jam sponsored by ABMP at the massagementorinstitute.com.
[music]
0:01:43.3 RW: Hi and welcome to I Have A Client Who: Pathology Conversations with Ruth Werner, the podcast where I will discuss your real life stories about clients with conditions that are perplexing or confusing. I'm Ruth Werner, author of A Massage Therapist's Guide to Pathology, and I have spent decades studying, writing about and teaching about where massage therapy intersects with diseases and conditions that might limit our client's health. We almost always have something good to offer even with our most challenged clients, but we need to figure out a way to do that safely, effectively and within our scope of practice. And sometimes, as we have all learned, that is harder than it looks. Before we begin today's story, I'd love to invite you to join me in moving our scapulae around just a little bit. Let's elevate them to bring our scapulae up to our ears, and then let's depress them and pull them down toward the sacrum.
0:02:50.2 RW: Let's protract them and roll them across and toward the front of our ribcage. And let's retract the scapulae and pull them back together toward the spine. And now let's just roll them every which way and enjoy that freedom of movement. And, haa, before we end, I'd like you to take a moment to abduct your humerae on both sides and get a great stretch as your scapulae rotate to allow you to do this. And now, I'd like you to think about what your life would be like if you couldn't do that. Today's I Have A Client Who story comes from a person who responded to my plea for more stories that I put out a couple of months ago, but they left me just a little bit of information and it was in the midst of a veritable tsunami of other great stories, so these two little sentences, they got lost, and I'm really sorry. And because of this, I never followed up with this contributor to get more information, and I have long since lost track of that person's name.
0:03:54.2 RW: So if you're listening, thank you so much for this story, and maybe you can get back in touch with me and tell me a little bit more about this client, like how old she is and if she'd had surgery and what the aftermath of that surgery might have been. In the meantime, we're going to forge forward with just this little bit of information, which gave me an opportunity to learn some new things for which I am always grateful. And our story goes like this. "I had one client who had Sprengel's deformity. She told me she could never get a massage or chiropractic care, but she found great relief from the few massages that I gave her." Okay, Sprengel's deformity. This turns out to be a congenital condition, that is, it's visible at birth or in very early childhood. Here's a quote from one of the resources that I have listed in our show notes. They say, "Sprengel's deformity is a rare congenital deformity of the shoulder girdle, characterized by a failure in the descent of the scapula to normal position during development, leading to a hypoplastic, elevated and mal-rotated scapula." Hmmm. So what causes this? Most cases appear to be random, rather than running in families. It has been identified as a problem with blood supply to the subclavian area during the 9th to 12th weeks of gestation, so that's pretty precise.
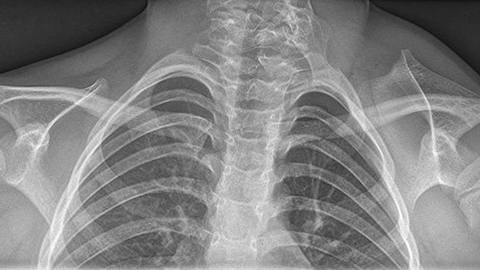
0:05:19.7 RW: And the consequence is that the scapula on that side doesn't form normally. And it might be hypoplastic, that is, smaller than a normal scapula. Remember hypo means below, and plastic means shape. It turns out that if this happens to the scapula, then hypoplasticity will probably also affect all the muscles that attach to that scapula. And there are a few other things that we see with Sprengel's deformity as well. This condition often appears with some other musculoskeletal abnormalities, including Kliplofile syndrome, scoliosis and spina bifida. Kliplofile syndrome is a new one on me. This is an anomaly in which two or more cervical vertebrae are fused, and this leads to a really shortened neck and a limited range of motion and pain. I have included an artist's rendering of an MRI taken from a person who had both Sprengel's deformity and Kliplofile syndrome, so you can see how these situations affect the shoulder girdle. And of course you will find that in our show notes. Sprengel's syndrome is rare.
0:06:27.9 RW: It occurs in about 0.3 of every 10,000 live births. I did the math, and that means that in the United States we see about 120 new cases every year. So it's not terribly likely that you will have a client with this situation, but this is still really interesting. It affects more females than males, at a ratio of about 3 to 1. It's usually unilateral, but somewhere between 10% and 30% of babies born with this have it on both sides. It happens on the left side more often than the right side. That might have something to do with how the developing fetus lies in the uterus. This congenital disorder of the scapula was first identified in 1863 by someone entirely different from Sprengel, but in 1891 this Dr. Sprengel reported four cases of it in rapid succession, and that's when his name became attached to this disorder. Sprengel's deformity occurs on a range of severity, and it's often referred to as grades 1 through 4, so a grade 1 version of this condition is barely noticeable. It doesn't substantially interfere with shoulder function, at least during childhood.
0:07:38.5 RW: Although, before we're done today, I'm gonna talk about a case where it was diagnosed quite late, and it is possible that she had a mild version in childhood that then got progressively worse, sort of while nobody was looking. At the severe end of this spectrum is grade 4 Sprengel's deformity, which involves very severe malformations. We have at least two inches of difference between the heights of the superior angles of the scapulae, and this often occurs with a condition called neck webbing. Now, I had never heard that term, neck webbing, before, so I looked it up, and it's kind of a big deal. This is a situation that's seen with a variety of congenital abnormalities. Sprengel's deformity is just one of them, and it can involve all kinds of things like excess skin and connective tissues that run from the scapulae to the neck, and these are quite visible. It makes the neck look really short, and it cuts down on range of motion. And if Sprengel's deformity is not successfully treated during childhood, then people may develop a condition called omovertebral connections between the superior medial angle of the scapula and somewhere on the cervical spine. And I can hear you from here, omovertebral, you ask?
0:08:56.8 RW: Yep, I asked that question too. The prefix omo, O-M-O, comes from the Greek word for shoulder. So you might remember we have an omohyoid muscle. That's a muscle that runs from the scapula to the hyoid bone, which is of course that bone at the top of the neck that is the base of our tongue muscles. So some people with Sprengel's deformity are at risk for developing these omovertebral connections, which to the best of my ability to understand act essentially as connective tissue bands that eventually calcify and become bone-like. In fact, some resources call this having an extra bone, an omovertebral bone. So take a moment and think about having a thick, dense, maybe even calcified band of connective tissue running from the superior angle of your left vertebra up to, oh, say about C4 or 5. And now with that dense bone-like tissue there, try rotating your neck or laterally flexing your neck away from that side or raising your shoulder or lowering your shoulder. And you can see what a problem this will be.
0:10:12.7 RW: Sprengel's deformity is treated when abduction at that shoulder is limited to under 110-120 degrees, or when the obvious asymmetry of the placement of the scapulae is about 2 inches or more different. The only treatment for Sprengel's deformity that I was able to find any information about was surgery. And what we have found is that this is likely to be most successful if the surgery is conducted on a child who is under 8 years old. There are several surgical approaches to this condition, but so far the research has not favored any one technique over any of the others. And because this is quite a rare condition, it's not the kind of situation where surgeons get a chance to practice a lot or to try new things. Also, the surgical procedure typically involves releasing the muscles at the top of the scapula and then affixing the lower pole or the inferior angle of the scapula to a rib or embedding it in some of the lower muscles. This involves cutting through a lot of muscles and reshaping the trapezius and dealing with the neck webbing, and you can imagine the amounts of scar tissue and limitation that are likely to develop even if this is done in a child who is quite young.
0:11:24.3 RW: And we can see that it's much worse and harder to get a good result the older a person is when they undergo this procedure. I'd like to read a quote to you from a case report that I found that I thought might be really interesting to share. It's about Sprengel's deformity that has a very atypical presentation. So here's the quote. A 63-year-old woman presented with a complaint of chronic cervical pain, computed tomography scan showed elevation and rotation of the left scapula, partial fusion of the C2 to C7 vertebrae, and cervical scoliosis. An abnormal osseous connection between the supramedial border of the scapula and the left lamina of the C6 vertebrae was also seen. Imaging findings were compatible with omovertebral bone with Sprengel deformity. Sprengel deformity is the gestational failure of caudal migration of the scapula to its normal position. Right, so this lady was 63 when her chronic cervical pain finally drove her to get an official diagnosis and what they found in her CAT scans was evidence of a deformity that had been there since she was born, but only now had gotten to the point where it was really severely interfering in her quality of life.
0:12:42.3 RW: All right, so what does all this mean for our client? Well, we don't really know because we don't know very much about this client. Let's assume that this person's an adult, but we don't know if their Sprengel's deformity was severe enough to require surgery. I'm going to assume that the answer to that is yes, it was, since this person was told that they must never receive chiropractic care or a massage. So someone somewhere along the line felt this person's shoulder girdle attachments were so delicate that they shouldn't receive manual therapy to that part of their body. And we know from the person who sent in this story that in fact this client did receive massage and they found it helpful. What are some of the decision points that you would look for if you had a client with Sprengel's deformity and a history of this really invasive surgery that essentially reshaped their whole shoulder girdle during childhood? Think about that for a moment. The main things I would be interested to know would be how long ago was their surgery, what are their long-term repercussions from that surgery, whether their Sprengel's deformity is associated with any of the other challenges that they have, and if they have to manage their situation with analgesics or muscle relaxants or other interventions.
0:14:00.5 RW: And I bet that if you and I were in a room together and I asked you to come up with a list of things you want to know about their Sprengel's deformity before you work with this client, with a little bit of time you'd come up with all those questions and more. Also, if our client is an adult and they had surgery during their childhood without a lot of follow-up procedures, which is typical, it is safe to predict that their scar tissue will be extremely stable and probably pretty restrictive. So the next thing we need to know, of course, is what their goals are for massage because Sprengel's deformity can lead to problems in range of motion at the shoulder and shoulder rotation and shoulder elevation and depression and so on. You can imagine, then, how this can also contribute to neck pain and back pain, and all of these things can reverberate through the whole body. If our client is not taking pain meds or muscle relaxants, and if their scar tissue is old and stable, can you think of any reasons massage might not be a good idea for them?
0:15:00.1 RW: I can tell you from my own point of view, I think this person is probably a great candidate for massage, as long as we are clear about those variables. I am really glad that the client in this story abandoned that early advice about avoiding massage and she found that massage could be really helpful to her. And I hope that this client can continue to receive that excellent care for the best use of her shoulder that it's possible to get. Hey everybody, thanks for listening to I Have A Client Who: Pathology Conversations with Ruth Warner. Remember, you can send me your I Have A Client Who stories to ihaveaclientwho@abmp.com. That's ihaveaclientwho, all one word, all lowercase, @abmp.com. I can't wait to see what you send me, and I'll see you next time.
[music]