A client has PAH—and not just regular PAH, he has advanced PAH. No, he’s not spitting expletives—he has pulmonary arterial hypertension, a chronic, progressive, and ultimately terminal lung condition. He loves massage, but his therapist is concerned about the risk that blood clots might play in his disease. And—guess what—he has a history of multiple blood clots in his lungs.
Is there a way to work safely here? Maybe, with the right information and careful choices about bodywork.
What is PAH? And will we be seeing more of it soon? Listen in for more.
Resources: 
Pocket Pathology: /abmp-pocket-pathology-app
Deborah Jo Levine, M.D. (2021) ‘Pulmonary Arterial Hypertension: Updates in Epidemiology and Evaluation of Patients’, Supplements and Featured Publications, 27(3). Available at: https://www.ajmc.com/view/pulmonary-arterial-hypertension-updates-in-epidemiology-and-evaluation-of-patients (Accessed: 20 July 2022).
Khan, A.W. et al. (2021) ‘Pulmonary arterial hypertension post COVID-19: A sequala of SARS-CoV-2 infection?’, Respiratory Medicine Case Reports, 33, p. 101429. Available at: https://doi.org/10.1016/j.rmcr.2021.101429.
Lannan, K.L., Phipps, R.P. and White, R.J. (2014) ‘Thrombosis, platelets, microparticles, and PAH: More than clot’, Drug discovery today, 19(8), pp. 1230–1235. Available at: https://doi.org/10.1016/j.drudis.2014.04.001.
Pulmonary Arterial Hypertension (PAH) (no date) WebMD. Available at: https://www.webmd.com/lung/pulmonary-arterial-hypertension (Accessed: 20 July 2022).
Tudoran, C. et al. (2021) ‘Evidence of Pulmonary Hypertension after SARS-CoV-2 Infection in Subjects without Previous Significant Cardiovascular Pathology’, Journal of Clinical Medicine, 10(2), p. 199. Available at: https://doi.org/10.3390/jcm10020199.


As a Certified Advanced Rolfer™, Til was on the faculty of the Dr. Ida Rolf Institute® for 20 years, where he served as Coordinator and Faculty Chair of the Foundations of Rolfing Structural Integration program. The author of the Advanced Myofascial Techniques textbook series (which has been translated into 6 languages), his regular Myofascial Techniques and Somatic Edge columns have been featured in Massage & Bodywork magazine since 2009, and (along with Whitney Lowe) he co-hosts the popular Thinking Practitioner Podcast. He is the Director of Advanced-Trainings.com which since 1985 has offered short, credit-approved professional trainings and certification for manual therapists of all types, in person and online.
Website: Advanced-Trainings.com
Email: info@advanced-trainings.com
Facebook: facebook.com/Advanced.Trainings1/
Instagram: instagram.com/tilluchau
YouTube: youtube.com/user/AdvancedTrainings
0:00:00.0 Ruth Werner: Til Luchau is pleased to invite you to two amazing opportunities. Come to Til's popular hands-on sciatica training as it makes its Zoom debut on August 12th. Get a full day of personalized tutoring, camera-on supervision, and permanent recordings in CE credit, all at an amazing price. Til's new A-T subscription gives unlimited access to a growing catalog of over 35 curated advanced myofascial techniques, Feldenkrais and zoga movement classes for body workers, for as little as $20 per month. Sign up now at Advanced Trainings dot com.
[music]
0:00:46.3 RW: Hey, I Have A Client Who listeners. Did you know I have a growing library of NCB-approved, one-hour, online, self-paced, continuing education courses that you can do any time, anywhere? Well, now you know. Current classes include, What's Next: COVID-19 Updates From Massage Therapists, and A Massage Therapist's Introduction to Pharmacology Part One, and brand new, A Massage Therapist's Introduction to Pharmacology Part Two. Classes are $20 each, and they confer one hour of continuing education credit. Wanna know more? Visit my website at ruthwerner.com and check it out. Be sure to sign up for my mailing list so you'll never miss a new class.
[music]
0:01:42.0 RW: Hi, and welcome to I Have A Client Who, pathology conversations with Ruth Werner, the podcast where I will discuss your real-life stories about clients with conditions that are perplexing or confusing. I'm Ruth Werner, author of A Massage Therapist's Guide to Pathology, and I have spent decades studying, writing about, and teaching about where massage therapy intersects with diseases and conditions that might limit our clients' health. We almost always have something good to offer, even with our most challenged clients, but we need to figure out a way to do that safely, effectively, and within our scope of practice. And sometimes, as we have all learned, that is harder than it looks. Today's episode is about lung issues, something that I, as a person who lives with a chronic cough, take very seriously. And while this condition that I'm describing is rare at present, it's the sort of thing we might be seeing more of as part of the aftermath of COVID-19, because it has already been seen in many patients, including those who had only moderately severe infections. And this all began with a short back and forth between me and our contributor, who did give me permission to share this. From the contributor...
0:03:03.1 RW: "I just finished your online CE class on the ABMP site regarding blood clots. I have a client with advanced pulmonary arterial hypertension, and I'm trying to understand if there are any contraindications for massage. His doctor okayed him for massage, and I'll definitely ask my client for permission to reach out to his healthcare team, as you suggest in your course. But I was curious if you've worked with clients who have PAH and have any experience or suggestions you can share, especially regarding what to be careful about. He's a very large man and has severe swelling in all of his extremities. He has shortness of breath and a lot of stress. Massage feels really good to him and also helps his breathing. It's pretty remarkable how different his breathing is from the time he comes in to when he leaves after his massage."
0:03:53.2 RW: I responded, "I have no direct experience with PAH. But I wonder if this person has a history with COPD or lots of pulmonary emboli or maybe pulmonary fibrosis, anything that might limit the function of blood vessels in his lungs. That could lead to a backup and pulmonary edema and excess pressure in the pulmonary artery, I believe. Regardless, it sounds like you're on the right track. I love that you've communicated with his doctor, and if you haven't already, it would be great to ask about clot risk. We have a fair amount of data about massage for improved breathing and quality of life for people with COPD and asthma. Between being able to relax tense muscles related to breathing, those poor scalings and intercostals, and just giving our client a break from stress, it's not surprising that your work would be well received. Obviously, massage isn't going to fix this problem, but anything you can do to give him some relief is great, for him, for his loved ones, and for his healthcare team."
0:04:54.0 RW: Then our contributor responded, "Regarding your point about COPD and pulmonary emboli, he did mention he has lots of clots in his lungs, and I have a couple of quick clarifications. One is, I haven't spoken to his doctor personally yet. The client told me verbally that his doctor had cleared him for massage and I've worked on him twice, but now that I've been learning more about PAH and blood clots, I'm no longer comfortable working on him without medical guidance. And the second one is, I talked the case over with the manager-owner of the massage studio where I work, and she asked me to reach out to him to request a note from his doctor. I haven't been able to connect with him yet, but when I do I will also ask him if he'd be okay with me contacting his health care team directly. If you're interested, I will let you know what I find out."
0:05:40.6 RW: This is Ruth. There are some rules about how we can appropriately communicate with a client's health care team. I'll be delighted to cover that in a future podcast, just give me a good prompt. Our contributor concludes, "It's such a sad and scary situation. I've never seen anything like it, so much swelling. The skin is tight everywhere. I love that massage helps him feel better, I just wanna make sure it's not dangerous for him." Then we chatted about how to ask some useful questions of this client's health care team in order to figure out some safety parameters for this client. But while I am fairly knowledgeable about many lung issues, pulmonary arterial hypertension, or PAH is new to me.
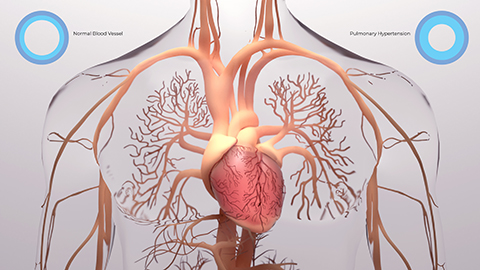
0:06:24.4 RW: I've found some good resources, which of course will be in our show notes, and here is a quick synopsis of what I have learned. Note, most of this information was gathered before 2019, so COVID was not yet a player. In those before times, PAH was a very rare disease, diagnosed between 500 to a thousand times a year total in the United States. It is seen most often in young women, which makes the client in today's story a little bit unusual. And because its presentation is not very consistent, it might be more common than we know, especially now in our new post-COVID population. PAH is defined as a group of severe pulmonary vascular disorders, in which pulmonary arterial pressure is higher than it should be when a person is at rest.
0:07:13.4 RW: What would that look like in someone who has it? Mainly we see the consequences of not having enough oxygen in the blood to meet the demands of muscles and organs. The most common early symptoms are poor stamina and weakness and shortness of breath and chest pain and fainting. These are pretty vague and it's easy to miss these signs or to attribute them to other problems. We might also see a cough, sometimes with blood, and as it progresses we might see an enlarged heart and liver and low blood pressure all over and hoarseness, and eventually puffiness, swelling in the face, the ankles, the abdomen and the feet due to edema. PAH has several subtypes. It can be related to connective tissue diseases, like lupus or scleroderma. It is an occasional but rare consequence of HIV/AIDS, or it could be completely idiopathic. One form is linked to the use of some drugs, including some appetite-suppressant drugs that were popular in the 1990s. Remember fen-phen? And sometimes, and possibly this is the situation with our client in today's story, it can be connected to a history of blood clots in the lungs. This can be called chronic thromboembolic pulmonary hypertension.
0:08:28.4 RW: In fact, there's a certain amount of controversy about whether blood clots cause pulmonary arterial hypertension, or if PAH triggers blood clots. It's probably circular and both, and this matters mainly to patients and physicians who are trying to determine the best treatment strategies. At this point, COVID is not listed as a specific contributor to PAH in the PAH information sheets, but a lot of data has been collected on the connection between these two conditions, and I would be surprised if we didn't soon see COVID added as a factor. No matter what causes PAH, it doesn't have a happy outcome. This is a chronic, progressive, and ultimately terminal disease. As the blood vessels in the lungs lose function, the right side of the heart has to work harder and harder to push blood into the lungs, and heart failure is almost guaranteed. That said, therapies now focus on preserving function and slowing progression as much as possible, and there are a number of options to do that. I just wanna remind us about the description of our client. Our contributor says, "It's such a sad, scary situation. I've never seen anything like it, so much swelling. The skin is tight everywhere. I love that massage helps him feel better. Just wanna make sure it's not dangerous for him."
0:09:50.5 RW: We don't know what kind of massage this person is providing. I'm going to guess that it is gentle and not demanding of a great allostatic adjustment or load. The client says his doctor has okayed him to receive massage. And you know how I feel about that. I did encourage this practitioner to follow up with a physician, to describe their massage and to ask specific questions about the risk of blood clotting. Which some resources say can happen outside of the lungs as well as within them. As I imagine this, the client is probably comfortable receiving only pretty conservative massage, and there might need to be some adjustments for how they lay on the table. With advanced pulmonary arterial hypertension and systemic edema, he's probably not able to exercise, which is both an important self-care strategy with people who have early stage PAH, and the ability to safely exercise is an indicator of the safety of massage, right? If someone is encouraged to exercise and get their heart rate up for a while, massage is unlikely to pose any greater stress than that to the cardiovascular system.
0:10:58.0 RW: And that just may not be in the cards for this client. So if this therapist can have a useful interaction with the physician to establish safety parameters, I can see that their work could be a welcomed, even treasured part of how this client invests in his self-care and quality of life. As I said in my correspondence with this practitioner, massage can't fix pulmonary arterial hypertension, but we can definitely be a joyful part of this person's life. So I really hope they're able to work with a health care team to come up with some good strategies for safe body work.
0:11:37.5 RW: Hey everybody, thanks for listening to I Have A Client Who, pathology conversations with Ruth Werner. Remember, you can send me your I Have A Client Who stories to ihaveaclientwho@abmp.com. That's ihaveaclientwho, all one word, all lowercase, @abmp.com. I can't wait to see what you send me, and I'll see you next time.
[music]