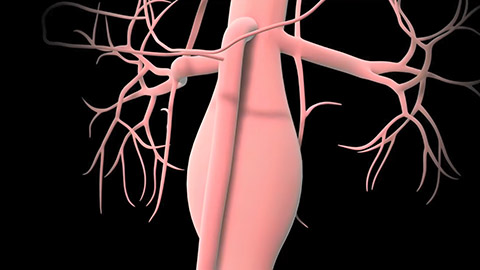
A client has a history of a triple A: an abdominal aortic aneurysm. If it ruptures, it has an 80% mortality rate. A few weeks ago, the client had surgery to correct another aneurysm, at her left subclavian artery—and this involved a 10 day hospital stay.
Is there any possible way that massage could be safe for this person?
Surprisingly, yes! Listen in for a great example of gathering the information we need to make good clinical decisions.
Resources: 
Pocket Pathology: /abmp-pocket-pathology-app


Anatomy Trains is a global leader in online anatomy educationand alsoprovides in-classroom certification programs forstructuralintegration in the US, Canada, Australia,Europe, Japan, and China, as well as fresh-tissue cadaverdissectionlabs and weekend courses. The work of Anatomy Trains originated with founder Tom Myers, who mapped the human body into 13 myofascial meridians in his original book, currently in itsfourthedition and translated into 12 languages. The principles of Anatomy Trains are used by osteopaths, physical therapists, bodyworkers, massage therapists, personal trainers, yoga, Pilates,Gyrotonics, and other body-minded manual therapists and movement professionals. Anatomy Trains inspires these practitioners to work with holisticanatomy in treating system-wide patterns to provide improved client outcomes in terms of structure and function.
Website:anatomytrains.com
Email:info@anatomytrains.com
Facebook:facebook.com/AnatomyTrains
Instagram: www.instagram.com/anatomytrainsofficial
YouTube:https://www.youtube.com/channel/UC2g6TOEFrX4b-CigknssKHA
0:00:01.2 Ruth Werner: Hey, I Have A Client Who. Listeners, did you know I have a growing library of NCB-approved one-hour online self-paced continuing education courses that you can do anytime, anywhere? Well, now you know. Current classes include what's next, COVID-19 updates for massage therapists and a massage therapist's Introduction to Pharmacology Part One, and brand new, a massage therapist's Introduction to Pharmacology Part Two. Classes are $20 each and they confer one hour of continuing education credit. Wanna know more? Visit my website at ruthwerner.com and check it out. Be sure to sign up for my mailing list so you'll never miss a new class.
0:00:48.0 RW: Anatomy Trains is delighted to invite you to our in-person Fascia Dissection Workshop, October 10th-14th, 2022. We're excited to be back in the lab with Anatomy Trains' author Tom Myers and master dissector, Todd Garcia, in Todd's Laboratory of Anatomical Enlightenment in Boulder, Colorado. Join students from around the world and from all types of manual, movement and fitness professions to explore the real human form, not the images you get from books. Visit anatomytrains.com for details.
[music]
0:01:33.9 RW: Hi, and welcome to I Have A Client Who Pathology Conversations with Ruth Werner, the podcast where I will discuss your real life stories about clients with conditions that are perplexing or confusing. I'm Ruth Warner, author of A Massage Therapist's Guide to Pathology, and I have spent decades studying, writing about and teaching about where massage therapy intersects with diseases and conditions that might limit our client's health. We almost always have something good to offer even with our most challenged clients, but we need to figure out a way to do that safely, effectively and within our scope of practice. And sometimes, as we have all learned, that is harder than it looks.
0:02:20.5 RW: Today's episode comes from a massage therapist who was able to provide a lot of detail, and this doesn't often happen in our I Have A Client Who stories, so I'm interested to take this deepest dive into arterial aneurysms and it goes like this. I wanna share my massage session I had today with you, the client gave me permission to share her story. I had a client who had just had subclavian aneurysm repair May 17th, 2022. The surgeon shut off the subclavian artery and re-routed the blood flow to the arm. This is all for her left side. A few years ago, she had a AAA. She said she has been diagnosed with a connective tissue disorder, but they haven't been able to give it a name. She wanted a massage because she was having some tension and discomfort in between her shoulder blades, especially on her left side. She also complained of her left arm feeling a little sore and feeling different, she said it's a similar feeling to how her legs felt for a while after the AAA.
0:03:24.7 RW: She had mentioned this to the surgeon and he did not seem concerned, she also said she was sore from her hospital stay in general because she was in there for about 10 days. She's 44 years old with no other health concerns, no medications besides a medication to keep her blood pressure low because of the potential for aneurysms. She has scans to check for other aneurysms, but at the moment she has none. Her heart is not affected by any of this. She has not been restricted for cardio, her only restrictions are for weight bearing at the moment. I felt with all the information I was able to go ahead and give the massage. She said she was able to and wanted to lay prone, I did offer to treat her side lying. I did a full body massage, but focused on her shoulder blades where she was having the discomfort. We agreed on having massage also to be relaxing as she has obviously been through a lot. I did work a little bit on the arm, particularly the triceps, when she's left, she said she felt so much better.
0:04:27.6 RW: She did mention the actual incision area has been feeling sore. I obviously stayed away from that area today, but I suggested she follow up with a surgeon about this and to also ask if she should have some physiotherapy to help with healing. I'm just writing to see if this would make a good episode, as this is the first time I have seen this in more than 10 years. I also wanted to know if I handled the situation well or if I missed anything. I actually am embarrassed to say this, but I'm not entirely sure how long to wait post-op for massage. I usually always just get the green light from the physio. I know there are studies to show benefits to receiving massage after surgery, but I'm just not sure of timeliness and I've been meaning to ask you for a while.
0:05:13.6 RW: Well, thank you, contributor. This is an awesome topic for an I Have A Client Who episode, and while you've never seen anything like this in more than 10 years of practice, the chances are good that you will never see it again, people with a history of multiple corrected arterial aneurysms are not that common. And you have provided lots of information to feed into your clinical decisions, and we'll come back to that in a bit. But first, of course, we get to talk about aneurysms, and I promise before we wrap up, we will talk a little bit about post-surgical timelines for massage. But here's a spoiler alert, it depends. So aneurysms, what are they? The word aneurysm has a Greek origin and it originally meant a widening or dilation, a perfect description of what's going on with these problems. An aneurysm is, simply put, a permanent wide spot or a dilation of a blood vessel, or in some cases, the heart itself. But how can a blood vessel or the heart develop a permanent site of dilation?
0:06:21.5 RW: Well, it's a combination of two factors, weakness or injury in the tissues, plus pressure. Lots and lots and lots of blood pressure. In the arteries, this isn't hard to picture, these are essentially three-ply tubes with delicate endothelium on the inside, a thick layer of muscle tissue in the middle, and a tough elastic outer layer of connective tissue. You remember these? The tunica intima, the tunica media, and the adventitia and with constant high blood pressure plus any damage related to atherosclerotic plaque, and of course these two things go hand-in hand, it is possible for an artery to develop a wide place in the road because of that combination of weakness and blood pressure. And if we remember that the heart is really just another part of the tubing as blood leaves the lungs and goes out to the rest of the body, we can see that the left ventricle, especially if it has a history of scar tissue from previous heart attacks, might also develop such a bulge.
0:07:24.2 RW: In this case of an otherwise healthy 44-year-old woman, we are probably not looking at someone with advanced heart disease, we're told she has an unnamed connective tissue disease that weakens her arterial walls. I know a couple of genetic connective tissue issues that can weaken arterial walls, Marfan syndrome and Ehlers Danlos syndrome both have a risk of arterial aneurysm among their possible complications, and there are probably other more obscure genetic connective tissue problems that do this too, and that may be what our client is living with. So aneurysms usually happen in arteries, especially the aorta and the cerebral arteries, because this is where blood pressure tends to be the highest, but they can also happen in the left ventricle, as we've mentioned, and this lady had one under her left subclavian artery, unusual, but not unheard of.
0:08:20.9 RW: It's rare, but possible for veins to develop aneurysms too, but the blood pressure in veins is much lower than in arteries, so these tend to not to happen without some other major thing going on, like a big trauma. And of course, the big risk with aneurysms is that they might rupture. If this happens with a cerebral aneurysm, we call this a hemorrhagic stroke or a brain bleed, and these don't have a great survival rate compared to the more common ischemic strokes. And in the case of aortic aneurysms, that doesn't bode well at all, most people will not survive a ruptured aortic aneurysm and this is why: When aneurysms are found, they are carefully evaluated and then possibly surgically repaired. I do wanna clarify that an aortic aneurysm can be small and stable and the risk of trying to repair it could be greater than the risk of what we call watchful waiting, that means scanning it regularly to see if it becomes larger. The surgery to repair aneurysms depends on where they are and how delicate they are. Aortic aneurysms can be repaired with open surgery and the insertion of a graft, or if the patient is a good candidate, they can be treated with endovascular surgery that uses a catheter in the artery to insert a graft into the damaged portion of the vessel.
0:09:45.9 RW: So let's return to the client in today's story. The surgery for her subclavian artery was just last May, this was just a few weeks before our contributor sent me this letter. I don't know if it was open surgery or endovascular surgery, but I will guess that since the client says the scar hurts and that she was in the hospital for 10 days, it was probably open surgery. We don't know what her procedure was for her AAA, by the way, that means Abdominal Aortic Aneurysm, but I'm willing to guess that that was probably endovascular, just given her general state of health and activity. Our contributor tells us she also complained of her left arm being a little sore and feeling different, she said it's a similar feeling to have her legs felt for a while after her AAA and she'd mentioned this to her surgeon and he did not seem concerned. She said she was sore from her hospital stay in general, she was in for about 10 days. That is a really long hospital stay, I don't doubt she was sore.
0:10:51.8 RW: We know she's 44 years old with no other health concerns, no medications, besides something to keep her blood pressure low because of her potential for aneurysms, she has scans to check for other aneurysms, but at the moment, she has none. Her heart is not affected by this, she has not been restricted for cardio exercise, her only restrictions are for weight-bearing, and this is all great information. Getting a sense of what is safe for our clients in terms of physical activity is a terrific guide to a person's tolerance for what massage might add to their other physical challenges. And knowing that this client is basically healthy only using blood pressure drugs and knowing it's safe for her to get her heart rate up suggest that there's nothing a 60-minute massage might do to be that overwhelming. Although it's always a good idea to find out about any side effects related to her blood pressure medications, because if they make her feel fatigued and loggy, we might wanna make adjustments for that. She wanted a massage because she was having tension and discomfort between her shoulder blades and especially on her left side and they agreed to have a massage to be relaxing as she's obviously been through a lot.
0:12:07.1 RW: Our contributor says, "I felt with all this information I was able to go ahead with the massage, I did a little bit on the arm, especially the triceps. When she left, she said she felt so much better. She mentioned the actual incision area has been feeling sore, I stayed away from that area today, I suggested that she follow up with a surgeon about this and also to see if she should have some physiotherapy to help with her healing." Our contributor asks, "I wanted to know if I handled the situation well or if I missed anything, I actually am embarrassed to say this, but I'm not entirely sure how long to wait post-op for massage." Okay, I think you will agree with me that this massage therapist did indeed gather all the needed information to work safely and conservatively with this client, especially with a focus on relaxation after that long hospital stay. There's just one piece of information I wish I had, which is about whether the subclavian artery surgery, the most recent one, had been an open procedure or an endovascular one, because that would have a big bearing on the size and location of her post-surgical scar.
0:13:13.5 RW: But the fact that she was in the hospital for so long suggests to me that this was an open surgery, which means the scar tissue is going to be a more important issue, of course. Our contributor asks for some guidelines about timing for post-surgical massage and he might be disappointed in my answer, because of course it depends. What does it depend on? Well, let's take a moment and list a few variables: How big and how deep is the scar, how old is it, is it fully healed or is it still delicate? Was there any post-surgical infection, how does it impact the client's range of motion, and what does that feel like? Does it feel like it's being stretched, or is itchy or achy, or is it giving you sharp cutting pain? Because all of these kinds of information might influence our choices.
0:14:01.4 RW: So here's a short reminder of what I know you know is safe: It is safe to work lightly in the neighborhood of a new surgical scar if the scar is covered and if we don't stretch the skin too far; and after the scar is fully healed and there's no more risk of infection, then manipulating that area within pain tolerance is safe and often recommended. We do have research to back this up. I won't try to list all of these in the show notes, but if you do a PubMed.gov search with the terms "surgical scar massage", you will see lots of information about this. There are other cautions around post-surgical massage and these would depend on things like what the surgery was for and if there was other kinds of tissue damage like the one people get their ribs cut open for heart surgery, or maybe there's a use of post-surgical drains or other devices that require us to accommodate this. So it's not possible to make other generalizations on this topic, but if this kind of information floats your boat, I do recommend that you look into scar tissue massage advanced education.
0:15:14.0 RW: I know for a fact that ABMP has a three-part online course by Nancy Keeney Smith and Kathy Ryan, that is excellent. So that's our story for today, we have a client who's prone to aneurysms, but otherwise healthy. We have a massage therapists who want some support for post-surgical decision making, and we have some new things for you to think about and that is a pretty good outcome for a 15-minute podcast.
0:15:41.1 RW: Hey everybody. Thanks for listening to I Have A Client Who Pathology Conversations with Ruth Werner. Remember, you can send me your I Have A Client Who stories too. Ihaveaclientwho@abmp.com, that's ihaveaclientwho, all one word, all lowercase, @abmp.com. I can't wait to see what you send me and I'll see you next time.
[music]