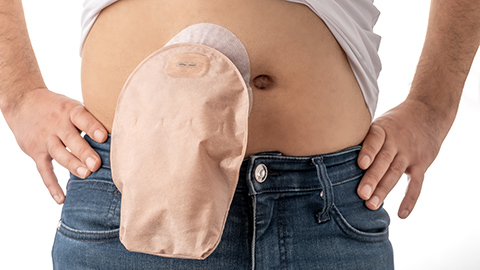
An older client has a complicated set of surgeries on her colon. Is it safe to receive massage?
It depends, of course. But what does it depend on?
Join us for this discussion of bowel resections, colostomies, and colostomy repairs—and find out one of Ruth’s very favorite pathology-related words. (Hint: it means “poop stone.”) Plus, there’s a really bad pun.
Resources: 
Pocket Pathology: abmp.com/abmp-pocket-pathology-app


This podcast sponsored by:
About Anatomy Trains:
Anatomy Trains is a global leader in online anatomy education and also provides in-classroom certification programs forstructuralintegration in the US, Canada, Australia, Europe, Japan, and China, as well as fresh-tissue cadaverdissectionlabs and weekend courses. The work of Anatomy Trains originated with founder Tom Myers, who mapped the human body into 13 myofascial meridians in his original book, currently in itsfourthedition and translated into 12 languages. The principles of Anatomy Trains are used by osteopaths,physicaltherapists,bodyworkers,massagetherapists,personaltrainers,yoga,Pilates,Gyrotonics,and other body-minded manual therapists and movement professionals. Anatomy Trains inspires these practitioners to work with holistic anatomy in treating system-wide patterns to provide improved client outcomes in terms of structure and function.
Website:anatomytrains.com
Email:info@anatomytrains.com
Facebook:facebook.com/AnatomyTrains
Instagram: instagram.com/anatomytrainsofficial
0:00:01.2 Ruth Werner: Hey I Have a Client Who... Listeners. Did you know I have a growing library of NCB approved one-hour online self-paced continuing education courses that you can do anytime anywhere? Well, now you know. Current classes include What's next? COVID-19 Updates for Massage Therapists and A Massage Therapist's Introduction to Pharmacology Part One, and brand new, A Massage Therapist's Introduction to Pharmacology Part Two, classes are $20 each and they confer one hour of continuing education credit. Wanna know more? Visit my website at ruthwerner.com and check it out. Be sure to sign up for my mailing list so you'll never miss a new class.
0:00:47.5 Speaker 2: Anatomy Trains is thrilled to announce our first ever Women's Health Symposium. This live online event takes place February 26 and 27, 2022 AWST, that's Australian Western Standard Time, register by January 21st to receive a significant early bird discount and over $400 worth of bonuses. We have invited a powerful line-up of all female authors, physicians, therapists and clinicians to share their passion and life's work. Visit anatomytrains.com for details.
[music]
0:01:35.9 RW: Hi, and welcome to I Have a Client Who... Pathology conversations with Ruth Werner, the podcast where I will discuss your real life stories about clients with conditions that are perplexing or confusing.
0:01:49.1 RW: I'm Ruth Werner, author of A Massage Therapist's Guide to Pathology, and I have spent decades studying, writing about and teaching about where massage therapy intersects with diseases and conditions that might limit our client's health. We almost always have something good to offer, even with our most challenged clients, but we need to figure out a way to do that safely, effectively and within our scope of practice, and sometimes, as we have all learned, that is harder than it looks. This week's episode comes from a massage therapist who found me online. They said they live in a rural area and have had a very sweet elderly client for many years. This client recently had a bowel resection and the massage therapist was interested to know about safety parameters for massage. When I asked for more information, I learned that this happened because the client had had diverticulitis and had had a type of ball repair, they removed the damaged section of her colon, but in the process, the client also needed a colostomy that was later reversed. This client is 75 years old, and the doctors have approved for her to receive massage, the only other incident she's had in the last year was a cornea transplant. Well, this sounds like a lucky client who has a caring and compassionate massage therapist.
0:03:15.1 RW: We could do a whole episode on diverticulosis and diverticulitis, and I'd love to if you'd like to send me your stories, but this therapist was asking more specifically about massage therapy in the context of someone who's had a bowel resection, which also involved a colostomy with a reversal. So that's what we're going to do.
0:03:36.3 RW: A bowel resection is a procedure in which a section of the bowel, usually the large bowel or colon is removed and the healthy ends are re-attached to each other. It's a pretty major surgery requiring full anesthesia and a hospital stay, it can be conducted as open surgery or laparoscopically or as robot-assisted surgery. These are done when something in the intestines, again, we're usually talking about the large intestine, seriously interferes with function. This could be a tumor or advanced scarring and stenosis, so fecal material can't pass through, it could be ulcerations like we might see with Crohn's disease or ulcerative colitis, or it could be uncontrolled bleeding. There are a few other things that can go wrong in the intestines, with intussusception and torsion and a couple of other things that might lead to bowel resections, but I've already talked about the most common situations. In the case of our client in this story, she had a different but also a common condition called diverticulitis, so we'll talk about that, but just for a moment. A diverticulum, the plural is diverticula, is a little pouch, and it hangs off the side of the colon, and lots of people get these as they get older and they are often related to weak musculature in the walls of the large intestine, so during peristalsis, the large intestine may bulge.
0:05:04.8 RW: The problem with these diverticula, is that they can harbor fecal material, it can just gather in there and stay. If that fecal material hardens and petrifies, this is sometimes called a fecalith, which literally means poop stone, one of my favorite words, ever. But more often, this material festers and creates a local infection with lots of inflammation and abscesses and a risk of scarring and spreading in really serious situations, this pouch, this diverticulum that's full of fecal matter and infectious material can rupture and of course, this can lead to peritonitis, which can be deadly. So the condition of having diverticula that's called diverticulosis may complicate into diverticulitis that is swollen diverticula. And if the situation is not controlled through antibiotics and dietary changes and other interventions, and especially if it gets progressively worse or there is a substantial risk of rupture and peritonitis, then it may become necessary to remove the part of the bowel that has been weakened and compromised and it sounds like that's what happened for this lady. In some bowel resections, the ends of the colon that remain are just attached to each other with sutures or staples, so everything can be completed in a single surgery.
0:06:28.3 RW: However, this lady needed a colostomy, that suggests that something was going on with the cut ends of her colon that might interfere with their healing properly. Colostomy, when we take that word apart, what we see is colon and stoma. A stoma is a mouth or opening. You're probably aware that in a colostomy, a person has a channel from their large intestine to an opening in their abdominal wall where fecal material drains into an external back. The person can empty the bag as often as necessary like right before a massage, for instance. The ostomy site where the two comes to the skin is important to keep extremely clean to reduce the threat of external infection. I've heard from some people that sometimes the ostomy is located within the abdominal fold, the place where the belly folds over on itself when a person is sitting, and that makes a problem because it is much harder to keep that area clean and dry, plus it's prone to a lot of friction and disruption. The bag is attached to the skin with an adhesive that can be weakened by oils or lotions, so it's important to keep that in mind for massage.
0:07:40.2 RW: Beyond avoiding the ostomy itself and where the bag is adhered to the skin, the only specific massage therapy accommodations that we need to make for someone with a colostomy will be guided by their comfort. They might prefer not to be face down, they might want to skip deep abdominal work, but warm comforting hands through the sheet would probably be delightful and welcome.
0:08:04.1 RW: And of course, other factors might have to do with why they needed the colostomy in the first place. Sometimes, as is the case for this client, colostomies are temporary, and they may be done in the context of bowel resections where there is some reason that the two ends of the resected bowel aren't unlikely to fuse together well. Bowel resections and colostomies are major surgeries, they involve hospital stays from 3-7 days, which is a lot, and months of recovery. They also carry some risks related to surgery in general, the possibility of hospital-borne infections, DVT and pulmonary embolism, leakage of fecal material into the peritoneum and inadvertent damage to other organs or nerves or blood vessels. However, most of the time, this surgery goes without major incidents and patients can look forward to a healthy and highly functional life for a long time into the future. But at this point, our client's colostomy has been reversed, that means she had additional surgery to re-attach the ends of her colon, and this usually happens several months or up to a year after the colostomy is created. This means she should now have an intact and functioning digestive tract, although it is shorter than it used to be, and I just can't resist this pun perhaps now instead of having a colon, she has a semicolon.
0:09:25.3 RW: Okay, so what about massage for this person? Does her history with diverticulitis or bowel resection or colostomy and reversal have any bearing on decisions about massage therapy? If you know me, you know my first answer to questions like this is, it depends. What does it depend on? Well, what do you think? I think it depends on how long ago was her last surgery, we don't have that information in this story, but we do know that her doctors feel massage is safe for her. That's great. But it's not enough information. I also wanna know is she taking any medication in relation to her diverticulitis or other GI tract problems and if yes, of course I'd like to know what that is and about what kinds of side effects she has. Does her surgery and resulting scar tissue limit her activities in any way? Does she have any lingering pain related to her diverticulitis or her surgeries? That's just the short list of questions that I came up with off the top of my head. You may have more like is she comfortable being face down on the table, how does she feel about massage to her abdomen and some others I'm not even thinking of yet, and of course, the most important question of all is, what does she hope massage can do for her today? I think this client is probably a great candidate for whatever kinds of massage she would like to receive, and I think she's lucky to have this careful and compassionate massage therapist for her provider.
0:10:51.9 RW: Have you had clients with colostomies that presented unexpected challenges? I know our listeners would love to hear about it, so please be sure to let me know and you could show up in a future episode of I Have a Client Who...
0:11:06.0 RW: Hey everybody. Thanks for listening to I Have a Client Who... Pathology conversations with Ruth Werner. Remember, you can send me your I Have a Client Who... Stories to ihaveaclientwho@abmp.com that's I have a client who all one word, all lowercase at A-B-M-P dot com. I can't wait to see what you send me and I'll see you next time.