Explain the Process as You Work Through It
Different avenues and various support helped one client battle the aftereffects of a stroke.
Exercise-related leg pain is a frequent complaint, yet few terms are as casually used—or misunderstood—as shin splints. There are two primary forms of shin splints: anterior and posterior/medial, also known as medial tibial stress syndrome (MTSS). Recent research has shifted our understanding of the causes and, consequently, our treatment strategies for these conditions. As with many lower extremity problems, the kinetic chain plays a prominent role in their development.
Here, we will explore anterior shin splints and MTSS and highlight other conditions to rule out. We will also address kinetic chain dysfunctions to treat the underlying causes rather than just the symptoms.
Both anterior shin splints and MTSS are issues of overuse or repetitive-use injuries; however, each presents differently.
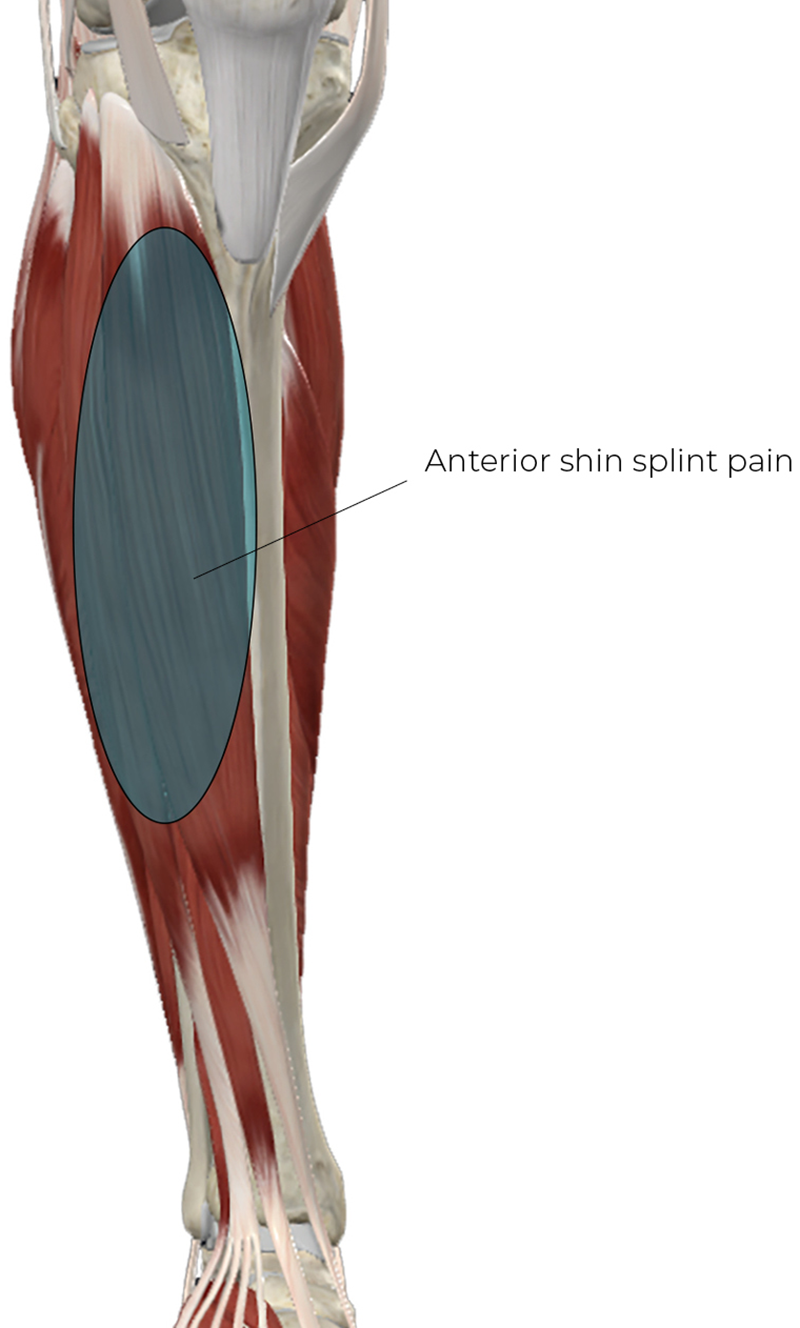
This condition involves pain centered over the anterior tibial shaft and muscle compartment, primarily affecting the tibialis anterior, extensor digitorum longus, and extensor hallucis longus (Image 1). Anterior shin splints are caused by activities requiring excessive dorsiflexion, such as downhill running. The dorsiflexors work eccentrically to control foot deceleration at heel strike to prevent the foot from slapping the ground. This often leads to the fatigue and soft-tissue irritation characteristic of anterior shin splints. This repetitive eccentric overload is the primary driver of this injury.
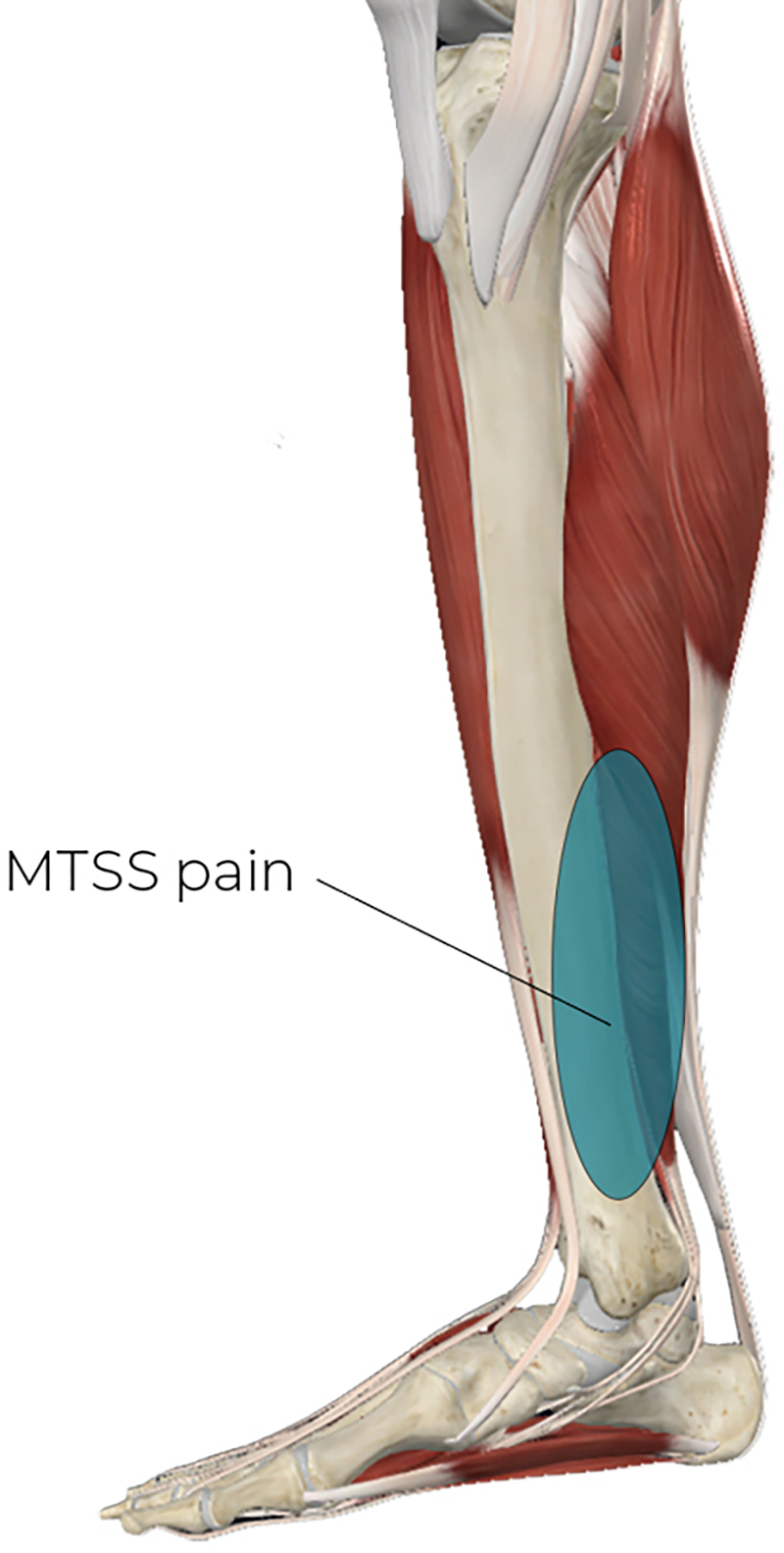
MTSS is the most common form of shin splints (Image 2). For decades, the periosteal traction theory held that deep posterior compartment muscles pulled on the periosteum, causing local inflammation. However, current research supports a bone stress-overload model. In this model, repetitive compressive loads (like running) outpace the tibia’s ability to remodel. Bone breakdown exceeds formation, leading to accumulated microdamage within the tibial cortex itself.1
The forces traveling through the lower extremity kinetic chain are important factors that can contribute to MTSS, including postural challenges. Weakness in the gluteal muscles (specifically gluteus medius and maximus) leads to poor pelvic stability. When the pelvis drops or the femur rotates internally during gait, the stress travels downward, significantly increasing the load on the tibia. These kinetic chain forces can also go in the opposite direction.
A postural distortion in the foot, such as overpronation, can cause an increase in the ground reaction force at each foot strike, which causes cumulative compression loading on the tibia and may lead to MTSS. If MTSS persists, it may eventually lead to a stress fracture. Following, I offer some ways to distinguish MTSS from a stress fracture.
Other lower-leg disorders can mimic anterior shin splints or MTSS, so accurate differentiation is crucial. Chronic exertional compartment syndrome (CECS), also called anterior compartment syndrome, is a distinct overuse condition and should not be confused with shin splints. It also should not be confused with acute anterior compartment syndrome—a medical emergency, usually caused by a direct blow to the lower leg that requires immediate referral. The term CECS is preferred to distinguish between these two conditions.
Compartment syndromes arise when intramuscular pressure climbs to dangerous levels during activity or after trauma. Both CECS and acute anterior compartment syndrome can produce neurological and vascular symptoms (numbness, burning, tingling, or coldness). The key distinction is that CECS is activity-related and typically resolves after stopping the aggravating exercise, whereas acute anterior compartment syndrome presents with rapidly escalating, persistent symptoms.
Our hands-on work is invaluable for improving tissue health and addressing the kinetic chain dysfunctions in the hips and feet that drive these injuries.
Massage is contraindicated during a CECS flare-up; once activity has ceased and swelling and symptoms have subsided, massage is generally considered safe. Persistent or acute neurovascular symptoms, as in acute compartment syndromes, always warrant urgent medical attention.
Evaluations narrow down which tissues are involved and need treatment. Knowing which tissues to address is necessary for effective treatment with these conditions. While massage therapists do not diagnose, a structured assessment is essential to rule out serious conditions whose treatment depends on referral to another health-care professional.
Taking a history is the cornerstone of evaluation. Begin by investigating the pain onset—specifically any recent spikes in training volume, activities, or a history of postural issues. Remember:
Anterior shin splints are often brought on by significant downhill running or walking.
MTSS often results in a dull ache in the distal medial tibial region.
Next, clarify the nature and location of the pain. Ask the client to pinpoint the location. Pain in the proximal, muscular portion of the tibia usually indicates anterior shin splints. Pain localized to the distal medial tibia is more indicative of MTSS, which is characterized by diffuse tenderness along the posteromedial border of the distal two-thirds of the tibia.
Gentle palpation differentiates these conditions with greater precision.
Anterior shin splints: Apply moderate pressure to the dorsiflexor muscles while the client performs resisted dorsiflexion. Pain reproduction during this maneuver strongly suggests involvement of the dorsiflexor muscles.
MTSS vs. stress fracture: Palpate the posteromedial tibial border to distinguish between these two conditions.
The 5 centimeter rule: MTSS typically presents as diffuse tenderness spanning at least 5 centimeters (about 2 inches).
Focal tenderness: If the client reports sharp, exquisite pain localized to a specific point smaller than a coin, this is a major red flag for a tibial stress fracture. In this instance, manual therapy to the area is contraindicated; refer the client for a comprehensive evaluation.
During evaluation, it’s essential to explore key biomechanical factors that play a role in shin pain (anterior or posterior) due to overuse.
Foot mechanics
Hard running surfaces
Hypertonic muscle patterns
Poor or improper footwear
Related kinetic chain relationships
Training errors
Our hands-on work is invaluable for improving tissue healing and addressing the kinetic chain dysfunctions in the hips and feet that drive these injuries. Effective treatment for both anterior shin splints and MTSS requires strategic progression from general to specific applications.
Before diving into deep, focused work, it is important to begin with broad contact gliding techniques. These approaches reduce general hypertonicity and downregulate nervous system irritability. By calming neural reactivity first, you create a more receptive environment for the targeted work needed for treatment.
Active engagement techniques are effective adjuncts to the treatments above. However, proceed with care. These muscles can present with varying levels of severity and pain, so it is vital to work within the client’s pain tolerance to avoid causing discomfort.
While it is a physiological myth that manual therapy techniques have the physical force to pull muscles away from the bone, change your approach, including direction and intensity, if any application causes too much pain.
Deep cross-fiber applications combined with active engagement are highly effective for addressing the anterior compartment. This approach allows for better penetration of your pressure and helps restore pliability and elasticity to the muscles. Use your thumbs or a broad contact surface, such as the heel of your hand, to apply cross-fiber broadening to the muscles with movement (Image 3, also see accompanying video).
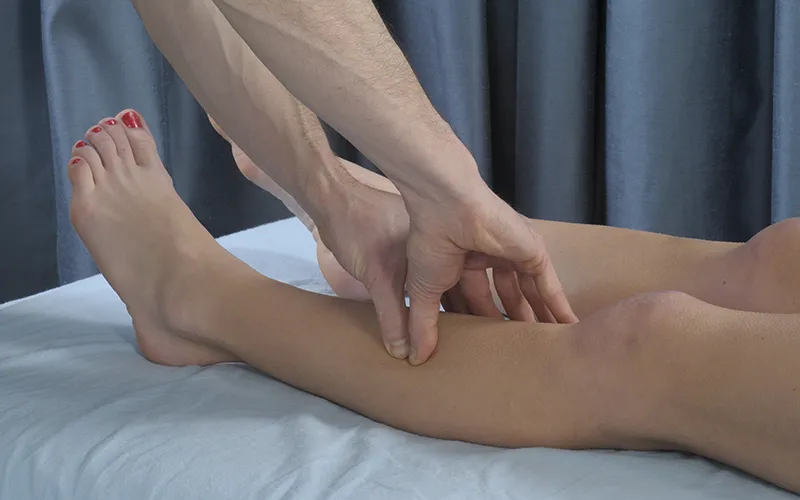
For this technique application, do the following:
First, demonstrate foot dorsiflexion and plantar flexion to the client. Have the client start at a slow, steady rhythm and maintain it throughout the treatment.
Simultaneously apply the cross-fiber stroke to the anterior compartment muscles as the client actively dorsiflexes the foot, shortening the muscle.
Pause your pressure as the client lowers their foot back into plantar flexion.
Perform the broadening technique again on the subsequent dorsiflexion. Gradually work your way up the length of the anterior compartment until the entire region has been thoroughly covered.
These techniques serve as an excellent follow-up to shortening movements and are highly effective for enhancing flexibility and reducing tension in the anterior leg muscles. The goal here is to perform a deep stripping technique while the muscle lengthens (Image 4, also see accompanying video).
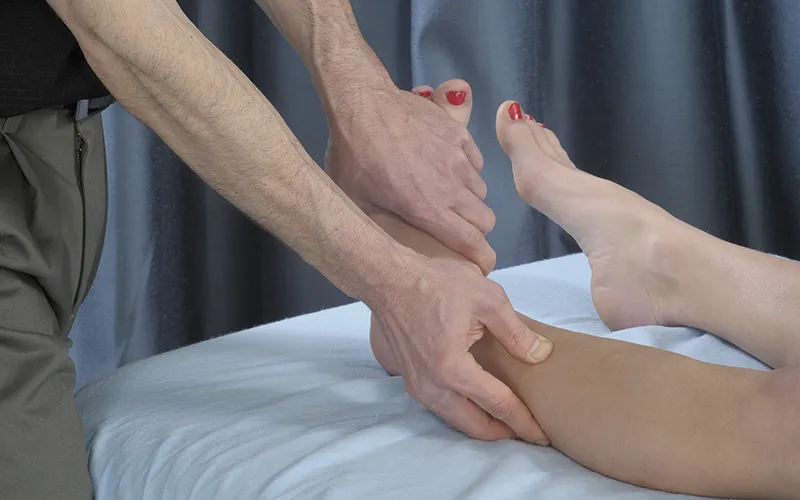
For this technique application, do the following:
Have the client bring their foot into full dorsiflexion.
Place one hand on the dorsal surface (top) of the foot to provide resistance.
Instruct the client to hold the position to engage the muscles isometrically.
Instruct the client to slowly release the hold, maintain your resistance at the top of the foot, and gradually push it into plantar flexion. Ensure the anterior muscles are working eccentrically.
Use your other hand to perform a longitudinal stripping technique along the length of the anterior compartment muscles.
For posterior leg treatment, both the superficial posterior compartment muscles and the deep posterior compartment (tibialis posterior) need to be tended to.
We can also apply active engagement used on the anterior leg to the superficial posterior compartment muscles: the gastrocnemius and soleus. Apply broad cross-fiber techniques during the shortening phase (plantar flexion) and longitudinal stripping during the lengthening phase (dorsiflexion).
The primary muscle that gets overworked in MTSS is the tibialis posterior. This muscle can be challenging to access, so active engagement is beneficial. The tibialis posterior is in the deep posterior compartment and is wrapped around the back side of the tibia. It is deep to the larger calf muscles, so if you don’t use a small contact surface right against the tibial border and press into this area, you will gloss over the muscle and not treat it.
To access these tissues effectively, place the client in a sidelying position with the affected leg resting on the table, medial side facing up. This position allows the best access to the medial tibial border and deep posterior compartment muscles (Image 5, see also accompanying video).
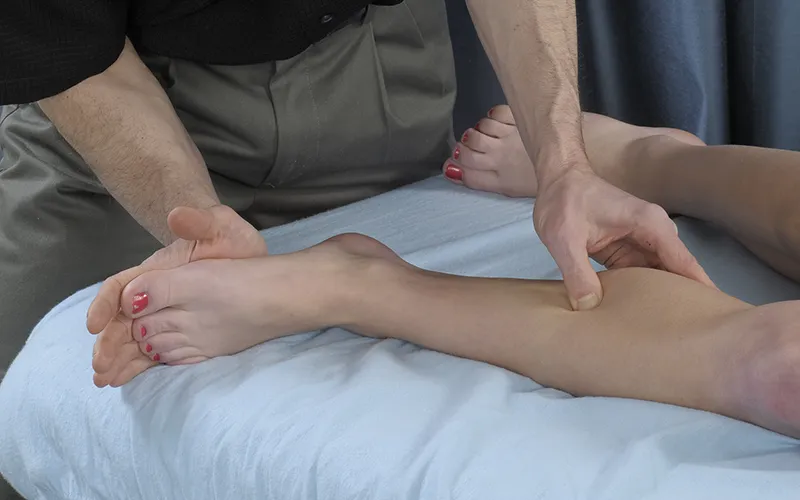
Work with caution, as this area is likely to be painful for the client, especially those with active symptoms. Communicate with your client regarding pressure levels to ensure the treatment remains within a therapeutic tolerance. For this technique application, do the following:
Instruct the client to repeat slow dorsiflexion and plantar flexion used in the previous active engagement technique.
Use your fingertips or thumb to gently curl behind the medial border of the tibia. You are aiming for the deep space between the tibia and the soleus muscle.
Perform the technique during the dorsiflexion phase. As the foot moves into dorsiflexion and the tibialis posterior lengthens, apply a slow stripping technique along the posterior tibial border using a small contact surface (thumb, fingertip, or tool).
Be careful not to press directly onto the periosteum (the bone surface). Instead, direct your pressure toward the posterior aspect of the tibia to engage the muscle tissue adjacent to the bone.
Let’s talk about relative rest. For these conditions to heal, the client must cease offending activities for a period long enough to allow the bone and tissues to heal. Relative rest does not mean complete bed rest. It means encouraging clients to maintain fitness through nonstressful activities, such as low-impact cross-training, swimming, deep-water running, or cycling.
Once the acute pain subsides (usually, pain-free walking is the first benchmark), they can begin a graded return to activity, meaning they can slowly increase training variables—distance, frequency, and intensity—over weeks (not days). If pain returns, they must regress.
Massage therapy has long been a go-to method for treating shin splints, both for high-level athletes and among everyday exercise enthusiasts. Our hands-on approaches are proven treatments for these painful and life-affecting conditions. We are also gatekeepers who, by recognizing when to refer out for stress fractures or compartment syndromes, can intervene to help prevent further injury to our clients, becoming not just muscle massagers but integral partners in our clients’ treatment.
Different avenues and various support helped one client battle the aftereffects of a stroke.
Caring for elderly clients requires the massage therapist to have a keen awareness, not only of the characteristics unique to the client but also of the various members of the client’s care team.
This variation of your massage stance can reduce discomfort, help conserve strength, and use your movement and body weight most efficiently during a session.
When focusing on stretching a target muscle, sometimes other muscles in the group need to be considered for the session to be effective.