Working with Clients with Hypothyroidism
Understanding hypothyroidism’s symptoms, causes, and treatments can guide MTs in better interacting with these clients.
This edition of Pathology Perspectives is a departure from my typical offering. I usually start with a description of some pathologic condition, and then go through demographics, etiology, and signs and symptoms, and I finish with implications for practice, often with a call to action for massage therapists. But in this article, we are going to take a very brief look at a subtype of squamous cell carcinoma, and then track in detail the progress of the condition and treatment with a person who has generously shared her story with us.
Squamous cell carcinoma (SCC) is cancer that affects the keratinocytes, just superficial to the basal layer of the skin. It is diagnosed in about 1 million Americans each year. Usually SCC lesions are simply removed with liquid nitrogen or a shallow incision, and no further treatment is needed. But in some circumstances, SCC has a potentially dangerous pattern that I had never heard of before I began developing this article: perineural invasion.
Perineural invasion (PNI) is a feature of a small number of cancers that affect the face and head. In this situation, cancer cells use motor or sensory nerves to travel and possibly metastasize to other locations. This pattern is almost exclusive to cancers that affect the face and head; most other forms of cancer use blood, lymph, peritoneal fluid, or direct contact to move to new locations.
PNI occurs in approximately 5 percent of diagnosed cases of SCC, and it is associated with an increased risk for cancer recurrence, local and distant metastasis, and a poor prognosis. PNI can be found in a few ways. The clinical presentation is that a person might describe symptoms of neuropathy: numbness, tingling, pain, or weakness in some area of the face. The histological pattern shows abnormal cells inside the perineurium (the wrapping around nerve cell fibers). One of the tricky things about PNI, however, is that it can cause "skip lesions"—that is, these depositions of abnormal cells are not necessarily continuous.
When SCC is diagnosed along with PNI, the treatment likely to yield the best outcome is Mohs surgery (a procedure that removes tissue in layers until a clear margin has been established), followed by radiation. Sounds simple, right? It isn't.
Perineural invasion occurs in approximately 5 percent of diagnosed cases of SCC, and it is associated with an increased risk for cancer recurrence, local and distant metastasis, and a poor prognosis.
If you are involved in the world of massage therapy or bodywork, it's safe to say that you have benefited from the work of Jan Schwartz. Jan is a former massage therapist, educator, and volunteer for numerous national and international organizations dedicated to massage therapy and integrated health care. The short list of Jan's volunteerism includes stints on the boards of the Massage Therapy Foundation, the Commission on Massage Therapy Accreditation, and the Academic Consortium for Complementary and Alternative Health Care (now the Academic Collaborative for Integrative Health). Jan was also the cofounder of online education provider Education and Training Solutions, LLC.
Jan is a mature, fair-skinned Caucasian woman. She grew up on the Jersey Shore, when laying out in the sun coated with baby oil was favored over the scrupulous application of SPF 90 sunscreen. She has lived in Tucson, Arizona, for 25 years, where she enjoys outdoor activities, including swimming, gardening, and hiking. All these factors: her age, a long history of sunburns, and current location and habits, put Jan squarely in the high-risk group for various types of skin cancer. For this reason, she has always been diligent about twice-yearly visits with her dermatologist.
Jan has a long history of minor skin cancer incidents. But about six years ago, she had lesions on her scalp that were first observed not by her or her dermatologist, but by her hairstylist. "You have some spots I've never noticed before," he said. "You might want to have them checked out." That remark led to more invasive treatment: Mohs surgeries on her scalp and forehead.

Her most recent bout with skin cancer was the most serious to date, and Jan—ever the educator—invited me to share her story, so that others might learn from her experience.
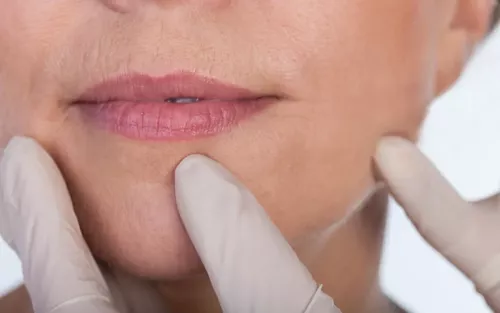
It began when Jan noticed a suspicious change in the skin close to the center of her upper lip in July 2017. She had a dermatology checkup scheduled for early August, so she didn't rush to make a new appointment. In fact, many of us saw Jan during that time, as we celebrated her retirement and many contributions to the profession at the Alliance for Massage Therapy Education meeting in Tucson.
But during that five-week period, she saw the lesion change rapidly. By the time she saw her dermatologist, it was a palpable bump of about a quarter-inch, with scaly, slightly darker skin than the surrounding area. It was not painful or itchy. It would have been easy to ignore or miss. But her dermatologist diagnosed it as a squamous cell carcinoma, a common type of skin cancer with a small-but-not-zero risk of metastasis.
Jan saw a plastic surgeon, who performed a Mohs-like surgery. The margins of the lesion were clear, and the surgeon was so skilled that the scar tissue was almost imperceptible: all in all, an excellent outcome.
But the following week brought some bad news. When Jan went to have her stitches removed, she learned that the analysis of the excised tissue showed signs of perineural invasion. This means the cancer could travel along nerve fibers from the skin and show up in other disconnected areas in the head or neck, including in the brain. The safest option was to follow surgery with radiation. Lots of radiation. Her oncologist predicted that 30 doses, given five times a week for six weeks, would probably take care of it.
When the time came to start treatment, a medical physicist (who knew such a specialty job existed?) determined the appropriate radiation dose, which had to be delivered with pinpoint precision. To achieve that, they made a mask: a flat piece of plastic mesh was heated and then put on Jan's face to conform to her shape as it cooled and shrank, a process that took about 45 minutes.
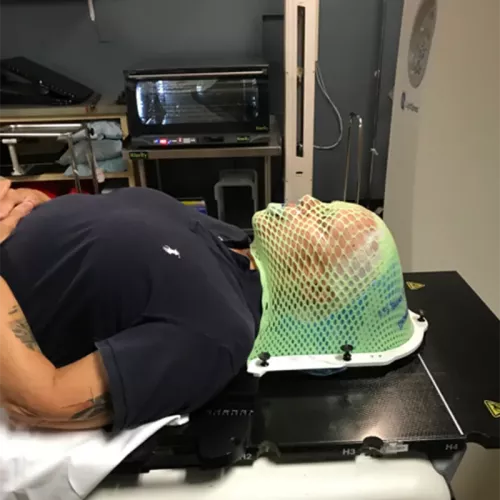
In some ways, making the mask was harder than the early radiation treatments: "It was the most horrible feeling to have your face, muscle by muscle, compressed," Jan says. "You can't move at all. I'm not claustrophobic, but this was really anxiety-producing. I could feel my heart racing, I was clenching and unclenching my fists. They told me they could stop if I needed, but then they'd have to start over from the beginning. I made it through."
After the mask was made, the radiation treatments were fast and efficient. The setup took about five minutes ("They have to bolt you down," Jan says), and the radiation itself lasted 40 seconds each session. Jan came through the first several appointments with flying colors and no big side effects.
After the 10th treatment, Jan noticed a tiny blister on the inside of her upper lip. By the end of the weekend, the blister had spread to the entire inside of her upper lip. Although the radiation doses were small, the burning continued to destroy cells even between treatments, and this was the result. Jan's medical team was surprised to see such severe blistering this early in the treatment series; although every person reacts differently, this was something they expected at the end of a six-week program, not in the middle. They persisted for another week—the halfway point—and by that time the pain was intolerable. The sessions were halted for a week.
Jan's lip was so swollen she couldn't talk or eat. She lost 10 pounds, and healing was slow. When it was time to resume treatment, they used a device called a bolus over her lip to limit the radiation scatter, and thus the collateral damage that was causing so much pain and tissue destruction.
Treatment number 30 finally concluded. It took two weeks for the swelling to subside, and several more weeks before the blistering cleared up. She couldn't brush her teeth throughout the whole process; she used special toothpaste in a dental tray. The fatigue that accompanies radiation was maddening, but slowly improved. "It's not the way I wanted to start my retirement," she says, "but it's good I had nothing else to do."
The pain of the blistering on the inside of her lip was intense. Oxycodone was helpful during the worst of it, making it possible to eat a little (mostly through a straw), so she could fight the fatigue and weakness. She used a mouth rinse with lidocaine, Benadryl, and Maalox to numb her lips so she could eat. Not surprisingly, everything tasted like Maalox for the duration of that intervention.
When salivary glands are exposed to radiation, they die. With less saliva in the key area, the blistering skin would frequently become glued to her top teeth—for weeks she essentially had to rip off the healing layers and start fresh every day. She couldn't touch her burned lip with her fingers, so she put shea butter or Aquaphor healing ointment on her lower lip to apply to the upper lip as best she could.
The complications of her cancer treatment became a profoundly emotional experience. Jan was frustrated with the pain that didn't seem to have an end in sight, plus a constant burning sensation on the outside of her mouth, along with crushing fatigue and the loss of the ability to eat without pain.
Now, several weeks later, Jan's mouth is mostly healed, but she still considers eating regular food a daily trial—and sometimes a triumph. She uses a Chinese burn cream on the outside of her lip. The affected skin is darker brown than the surrounding area, and it feels dry, swollen, and immovable "like an accordion that is stuck shut." It is safe to touch her lip, and although it is painful to manipulate it, she does so regularly to work on improving the quality of the tissue.
Jan's last follow-up appointment was positive. Her oncologist is confident that the cancer has been stopped, and she has a clean bill of health. In the meantime, she has no facial hair in the radiated area, and her salivary glands may never recover. But this won't slow her down. In the coming year, she and her partner plan to travel to Mexico, Israel (conditions permitting), Denmark, Sweden, Norway, and England. Jan is a devoted lover of life, and thanks to her diligence and her health-care team, she has a lot more to enjoy.
Massage therapists have a unique privilege: we see more of our clients' skin than they do themselves, and with regular clients, we see that skin over the course of time. With that opportunity comes a responsibility: we need to inform our clients when we see something that might require some attention. How we bring it to their attention is the tricky part.
I love what Jan's hairstylist said. How simple, how ordinary, how lifesaving! In the years that I have been a pathology educator, I have heard from many massage therapists with their versions of this story: a time when they recognized something on their client's skin and it turned out to be an important finding.
A couple of research studies highlight that the medical field appreciates our role as "first responders" in the context of skin cancer. But this role requires that we become deeply familiar with the forms and presentations of this disease, and that we become as comfortable as possible with expressing our concerns, while staying within our scope of practice. It is not appropriate to say, "Wow, sure looks like a big basal cell carcinoma here!" when we massage someone's scalp, but if we see or feel a suspicious change in the tissue, it is appropriate—and important—to say something like, "I notice something here that you might want to show your doctor."
How do you start this dialogue? Do you need some practice with a willing colleague? When this issue comes up, as it inevitably will, I hope you conduct these conversations with compassion and courage. What you say could save a person's life.
By John Otrompke

Learn more at www.theworldskinproject.org.
This is a facial rash characterized by its shape: the middle part of the butterfly is on the bridge of the client's nose, with "wings" extending onto the cheeks. "It can signify a range of diseases, from milder conditions like rosacea, significant acne, eczema, and psoriasis, all the way to serious autoimmune connective-tissue disorders such as lupus," says Joseph Jorizzo, MD, professor and founding chair of the dermatology department at Wake Forest University School of Medicine in Salem, North Carolina.
2. Infections
"Bodyworkers should look for any sign of infection, such as a cold sore, which is characterized by a painful bump or blister on the face or nose," says Jill Weinstein, MD, instructor of clinical dermatology at Northwestern University in Chicago. "This may be caused by herpes simplex."
Both viral and bacterial infections may appear as pustules or tender lesions. They can sometimes look like acne, but may also be bigger or more isolated than a pimple, Weinstein says. While a doctor referral is not always required for these conditions, you should avoid touching the areas in question so the infection is not spread to other parts of the client's body, to yourself, or to other clients.
MTs should be alert for round, patchy areas of hair loss that can be a sign of an autoimmune disease called alopecia areata, Jorizzo says.
"Alopecia is associated with thyroid disease, but it can also be upsetting to the client in and of itself," Jorizzo explains. "The prognosis is very good if there is just one little circle, but if clients lose their eyebrows or eyelashes, or if it goes around the bottom of the scalp, the condition is more likely to be chronic."
A client's nails may also offer evidence of a medical condition to the alert bodyworker. "Signs on the nails include a condition called clubbing, where there's body under the cuticle that changes the angle of the nail, so that it's like an upside down V," Jorizzo says. Clubbing is sometimes accompanied by edema, and the cuticle area may feel wet. It can be a symptom of several lung conditions, ranging from chronic bronchitis to lung cancer.
Pits in the nails can be a sign of arthritis or psoriasis. Pits resemble a mere dent, perhaps 1 millimeter across. Jorizzo explains, "In psoriasis, the outer layers of skin turn over very quickly, and when they come from under the cuticle, little patches fall off, so you get a pit."
Finally, a single dark black streak in the nail that comes up on to the cuticle can be a sign of melanoma.
The most common cause of skin cancer deaths is melanoma, which may be identified using the ABCDE criteria (see Spotting Melanoma—ABCDE Danger Signs, above), but the most common form of skin cancer is basal cell carcinoma. There are also some less common varieties that have different symptoms.
"Basal cell carcinoma often presents in the form of shiny or pearly bumps, which patients think are pimples," says Elizabeth Quigley, MD, a physician in the dermatology service at Memorial Sloan-Kettering Cancer Center in New Jersey. If the lesion has been there for six months, and sometimes bleeds, that's a warning sign that it is not a pimple.
Merkel cell carcinoma is typically seen in the elderly, or those who have problems with their immune system. "It often looks like a big red bump, usually greater than 5 millimeters, and usually rapidly grows over a period as short as a few weeks," Quigley says.
Atypical fibroxanthoma is another skin cancer found primarily in older individuals. "There are bumps, and the skin is colored redder than your normal skin," Quigley says. "The tumor is rapidly growing, with bleeding and persistent symptoms."
Squamous cell carcinoma, responsible for about 20 percent of all skin cancer deaths, has symptoms that are quite different from those of melanoma. "Squamous cell carcinoma can present as firm bumps, scaly patches, or ulcers that don't get better. The skin is red and the scale is the kind that doesn't go away with moisturizer," Quigley says. "It's different from just dry skin, and the scale is usually thicker." She says squamous cells don't rub off like normal dry skin, and the scaly patch may bleed if it is removed by pulling or picking.
Remember this list of danger signs for moles. Any of these symptoms could be indicative of skin cancer.
A more informal method of spotting a suspicious mole is called the Ugly Duckling test: when a mole just seems to catch your attention for some reason. "The classic example is when a client has one thing on her that just doesn't look like any other spot on her body," explains Elizabeth Quigley, MD. "Let's say she has many black moles, but one brown mole. Or most of the client's moles are round and small, but one is big and a different shape. That is a client who should be evaluated by a physician."
When you see something suspicious on a client's skin, how do you bring it up? "I usually phrase it like, 'I see this mole has an irregular shape. Have you noticed that?'" says Kirsten Kayser, a licensed esthetician and massage therapist in Denver, Colorado. "They may say yes or no. Then I say, 'Do you have a dermatologist that you like to see?' If not, then I say, 'Because I'm not a physician, I can't make a diagnosis, so I'm going to give you the name of a dermatologist who can check this for you, just to be safe.' I've had clients who were diagnosed with skin cancer after I referred them to a dermatologist. If I hadn't referred them, it could have been life-threatening."
It's natural for a client to ask what you think the problem is, but avoid answering that question. "I tell them, 'Usually it's nothing to worry about, but it's better to have it checked out,'" Kayser says. "Dermatologists can be booked months in advance, so I let the client know that they should call within the next couple of days to set up an appointment. It's also important to make a note in their file about what you found and who you referred them to."
What about those delicate situations where you need to refuse service because the client has an infection or otherwise problematic skin condition? Susanne Schmaling, a licensed esthetician and director of education for Associated Skin Care Professionals, says, "I never get specific about the disease, but describe the characteristics of what I see. If I have to refuse service due to open lesions, irritation, infection, or other unusual appearance of the skin, my statement is, 'I am concerned that I will cause this infection (or rash, or whatever) to get worse if I work on this area today.' You can also suggest an alternative if possible, such as a relaxation massage avoiding that part of the body."
Understanding hypothyroidism’s symptoms, causes, and treatments can guide MTs in better interacting with these clients.
Clients who have had head injuries can most benefit when their massage therapist makes them feel safe.
It's important to know the slight differences between fainting (syncope), and feeling faint, dizzy, or lightheaded.
While manual therapies do not stop the progression of Alzheimer's disease or dementia, they can help improve the patient's quality of life.